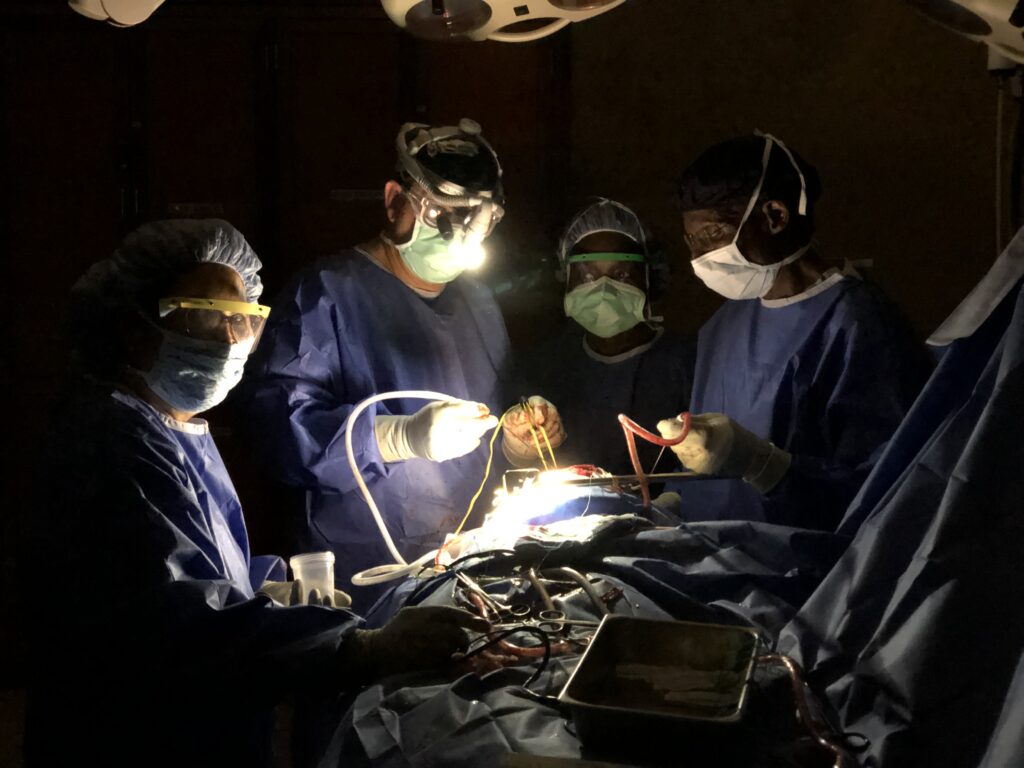
What matters? This is what I believe matters: “To whom much has been given, much more will be required” (Luke 12:48). As a neurosurgeon, I believe I have been given much; now, how do I give back? Paul Farmer’s statement, “The idea that some lives matter less is the root of all that is wrong with the world,” rings true, especially in low and middle-income countries with the greatest neurosurgical care disparity (Meara et al., 2015). In 1962, Great Britain gifted Uganda, which had gained independence, a brand new 1,500-bed hospital. Starting in 2007, on our first trip to Uganda, we found a country decimated by civil war, instability and poverty. The Mulago National Referral Hospital was a shell of its former self with no equipment, decrepit facilities and minimal operating room capacity. Dr. Jovan Kirybwere left Uganda to train in England, but unlike many trainees from Uganda who did not return, he knew “what mattered” and returned to his home country to become Ugandan’s first neurosurgeon in the 1970s. When his son, Joel Kiryabwire, wanted to become a neurosurgeon, Jovan Kiryabwere would have liked to train him in Uganda. However, the facilities were not up to standards, so he was sent to Australia. The elder Kiryabwere described his vision of training Uganda neurosurgeons in Uganda in a 1991 AANS video interview. On the initial trip to Uganda, we found missing in the operating rooms: Anesthesia machines, monitoring for oxygen, drills and bipolar cautery. Our philosophical approach involved twinning, technology, training and research (3TR). Twinning aims to improve everyone’s skills by pairing the Duke Neurosurgery and Neurology team (DGNN) with the Ugandans. Looking back, 17 years has involved 23 trips to Africa, with an average of 25 medical professionals on each team donating more than 40,000 hours of time. The technology transfer through the Duke PLUS (Placement of Life-giving Useable Surplus) transformed the operating and recovery rooms and the intensive care units at three neurosurgery hospitals in Kampala and Mbarara. We have transferred more than 14 tons of equipment and supplies worth $15 million USD to Uganda.
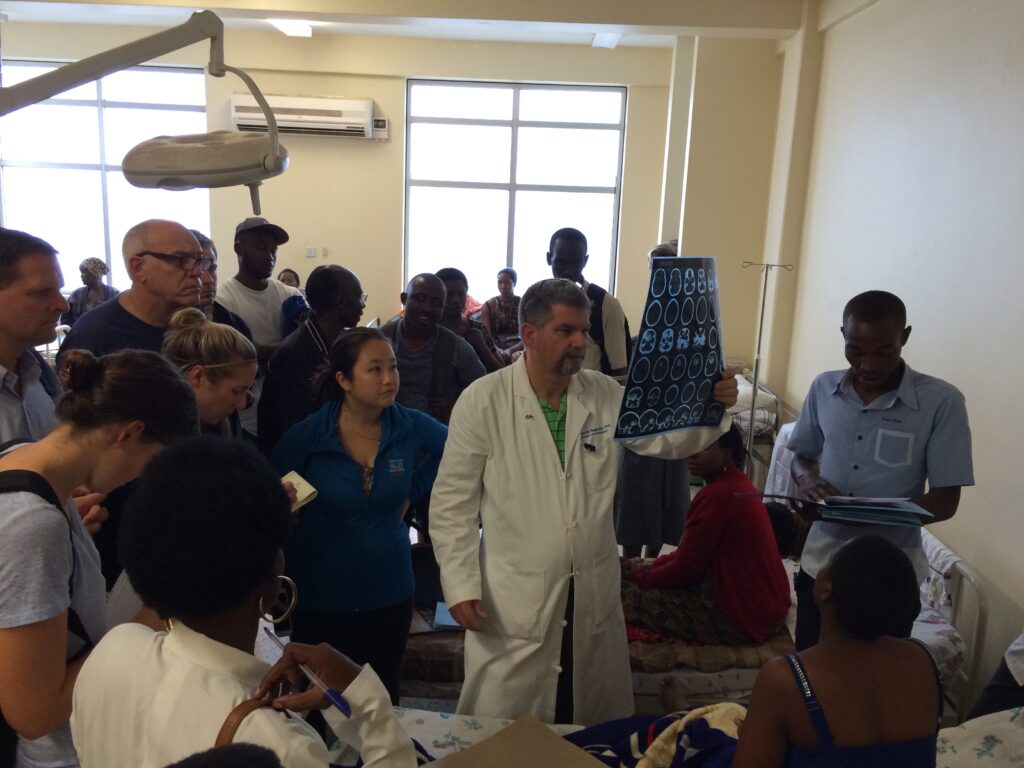
The training portion of the program started in 2009 with the help of Moody Qureshi, Paul Young and Robert Dempsey (FIENS). The COSECSA Neurosurgery Fellowship program was developed with Uganda, Tanzania, Ethiopia and Kenya. At the beginning of 2007, there were only five neurosurgeons in Uganda: Four at Mulago National Referral Hospital and one at the amazing CURE Hospital established by Ben Warf. Since 2009, nine neurosurgeons have been trained in Uganda and there has been no “brain drain.” These amazing individuals include the first woman neurosurgeon in Uganda, Juliet Nalwanga, with a pediatric neurosurgery fellowship at Toronto Sick Children’s Hospital. There are 22 more neurosurgeons in the training programs, with a goal of 63 by 2030. Professor David Kitya leads the second training program that just started at Mbarara. Traumatic brain injuries represent 77% of the neurosurgery operations performed. The 63 neurosurgeons will each train six general surgeons in treating traumatic brain injury to reach our goal of more than 400 neurosurgery trauma surgeons, making the dramatic increase in the ratio of surgeons with neurosurgery trauma expertise from one to six million (2007) to one to 140,000 (2030). There are other collaborative training programs on the continent with Cornell in Tanzania (Roger Hartl), Ethiopia (Knut Wester, Ruby Mahesparan, Morten Lund-Johansen) the new Barrow Global effort in Moshi Tanzania led by Dilan Ellegala, Kerry Vaughn and Cyrus Elahi). There are other outstanding efforts on the continent that are doing the twinning consistently, which I believe is critical for the full development of Neurosurgery in Africa; space limitation prevents mentioning all of these.
We started with “what matters,” there has been slow, steady progress in Uganda with twinning, technology, training and research. Lao Tzu stated, “Give a man a fish, and you feed him for a day. Teach him how to fish, and you feed him for a lifetime.” This is the vision for the Uganda Neurosurgery program. The progress from the Ugandan neurosurgeons performing complex tumor resections to running their own two-week neurosurgery camp has been amazing; the Ugandan surgeons know how to fish. In February of 2023, I was humbled to be an invited speaker at the first Neurosurgery Society of Uganda Meeting. Our final goal, which would complete the entire program and lay a solid foundation for the future, would be to build the Uganda Neurosurgery Institute: A dedicated neurosurgical hospital with an ICU, regular ward, rehab center, clinic and educational facilities. One of my secular philosophies is “Go Big or Go Home.” it was turned on me by the Minister Of Health when I showed her the fly-through of the hospital we hope to build. She said “Professor Haglund, we would like you to go big and build this hospital for us and then literally go home and let us take over with our greatest gratitude.”
Michael M. Haglund, M.D., Ph.D., MACM, FAANS,
Distinguished Duke Professor of Neurosurgery, Global Health, and Orthopaedic Surgery,
Vice Chair of Education, Duke Department of Neurosurgery,
Division Chief, Duke Global Neurosurgery and Neurology,
Professor SingHealth Duke-NUS Global Health Institute,
Adjunct Professor Barrow Global, Barrow Neurological Institute,
Program Director, Uganda Neurosurgery Training Program,
Duke Health,
Duke University