A Dire Situation
Afghanistan has been engulfed in conflict for over 40 years [1]. With the collapse of the government and freezing of national monetary assets in August 2021, the health system has seen a catastrophic regression and remains on the brink of collapse to this day, continuing to rely on humanitarian aid for its sustainment. In addition, single-use equipment has been in short supply due to international sanctions that limit the flow of medical equipment into the country. Despite numerous efforts to enhance health care infrastructure, a significant portion of the Afghan population still lacks access to safe, timely and effective surgical care [2].
This shortfall is particularly stark in specialized surgical fields such as neurosurgery, and is made even more difficult to address due to the ongoing political restrictions that limit the flow of people and equipment into and out of the country [3]. In addition, epidemiologic data on neurosurgical diseases in Afghanistan is scarce. Reports of neurotrauma have surged following the withdrawal of the U.S. military and subsequent political destabilization [4]. With only an estimated 74 neurosurgeons distributed across 16 primarily urban hospitals, the capacity to address these issues is severely limited [5].
Capacity Building Efforts
Current efforts to support neurosurgery in the country address various aspects, including governance, education, infrastructure and resources. Our team recently conducted the first assessment of neurosurgical capacity. We found that approximately 78% of the country is located within two hours of the 16 neurosurgical centers that are located in urban areas. These centers are overworked with only 74 neurosurgeons for a population of approximately 40 million – one neurosurgeon for every half a million people. Due to this limitation, many neurosurgical subspecialties such as pediatrics are lacking. With such a great need for clinical care, there is a lack of time and resources for academic pursuits, leading to a significant lack of neurosurgery research, with only 15 relevant papers published in searchable indices [5].
To overcome these challenges, we have followed the frameworks set forth for National Surgical, Obstetric, and Anesthesia Planning development and Kotter’s eight-step change model. In conjunction with performing our situational analysis and baseline assessment, we engaged stakeholders including neurosurgical leadership in Afghanistan, Ministry of Health representatives, global neurosurgery leaders, and members of the Afghan diaspora. We were able to re-establish the Afghan national neurosurgical society and assist them in joining the World Federation of Neurosurgical Societies (WFNS). Through the dedicated efforts of our neurosurgeons, we were able to host the inaugural Afghan National Neurosurgical Conference – in Afghanistan, a platform for local neurosurgeons to share their experiences and knowledge. To this day, we continue to grow our stakeholder base in a grassroots effort for building neurosurgical capacity. The rise of virtual online meetings was crucial to the success of our efforts as time constraints, travel restrictions and security concerns limited in-person meetings for stakeholders. Recognizing the challenge of unstable internet connections, we partnered with Afghan Wireless to install reliable internet and ensure a stable electrical supply at our partner hospitals, enhancing the engagement of Afghan doctors in training and telemedicine support.
Understanding that education is at the heart of our mission, we initiated short-term training programs, including sessions in neighboring countries, and long-term residency training abroad. We successfully sent four physicians for neurosurgical residency training in Spain, Italy and Pakistan, three of whom are women. We conduct weekly online educational sessions and actively promote telemedicine among surgeons. The integration of smart surgical glasses like Ohana One in the surgical field have also been a transformative tool. These innovative devices offer a range of functionalities that can significantly enhance the practice of medicine, particularly in challenging environments where resources may be limited. Using the glasses in Afghanistan, we have managed to assist on nine neurosurgical cases in remote areas of the country. Such technology further enhances these interactions, providing a platform for remote learning and expert guidance for Afghan health care professionals that might otherwise be inaccessible. Based on our initial needs assessment as well as the input of our Afghan colleagues, we have donated equipment (ten cranial sets, ten spinal sets, and six drills) for our colleagues to conduct surgeries.
To support these initiatives, we launched a fundraising campaign focused on various aspects of the project, including equipment donations, capacity building, partnerships with local stakeholders and specialty training, such as for endoscopic third ventriculostomy. The international Afghan diaspora has been instrumental in supporting these initiatives. It takes a village to undertake these endeavors, and we have found no lack of enthusiasm from the community for helping those suffering back in Afghanistan. Our initiative has been supported by the American Afghanistan Community Organization (AACO), World Federation of Neurosurgical Societies and Neurokids.
Challenges and Opportunities
Our efforts have faced numerous challenges, including the limitations in research and data, and reliable internet connectivity. Due to the international sanctions and restrictions on visas and commercial flights, it has been a challenge to find safe, affordable and reliable ways to send equipment into the country, travel to the country for trainings and bring Afghan neurosurgeons to other international centers for training. Over the past three years, Afghan citizens have faced significant challenges in obtaining visas for many countries due to the lack of international recognition of the Taliban government. Afghan diplomatic missions abroad, passports, visas and other documents issued by the previous administration are no longer honored. This has led to increased difficulties for Afghans seeking to travel internationally, as well as for our projects, causing delays and complications in securing visas for our neurosurgeons to attend training abroad [6].
Despite these challenges, we believe that local, regional and international efforts, combined with recent advancements in technology and telemedicine, will alleviate these issues and lead to significant improvements in the current situation. There is a tremendous opportunity for growth and impact on the lives of innocent Afghan citizens. We continue to look for partners in our endeavors and always welcome support.
References
1. Spagnolello, O., et al., Civilian war victims in Afghanistan: five-year report from the Kabul EMERGENCY NGO hospital. European journal of trauma and emergency surgery, 2023. 49(3): p. 1401-1405.
2. Contini, S., et al., Emergency and essential surgical services in Afghanistan: still a missing challenge. World journal of surgery, 2010. 34: p. 473-479.
3. Park, K.B., W.D. Johnson, and R.J. Dempsey, Global neurosurgery: the unmet need. World neurosurgery, 2016. 88: p. 32-35.
4. Reger, M.A., L.A. Brenner, and A. du Pont, Traumatic brain injury and veteran mortality after the war in Afghanistan. JAMA network open, 2022. 5(2): p. e2148158-e2148158.
5. Ammar, A., et al., The current state of neurosurgery in Afghanistan. World neurosurgery, 2023. 169: p. 110-117. e1.
6. Albrecht, C., B. Rude, and T. Stitteneder. Afghanistan’s free fall–return of the Taliban and flight as a last resort. in CESifo Forum. 2021. München: ifo Institut-Leibniz-Institut für Wirtschaftsforschung an der ….
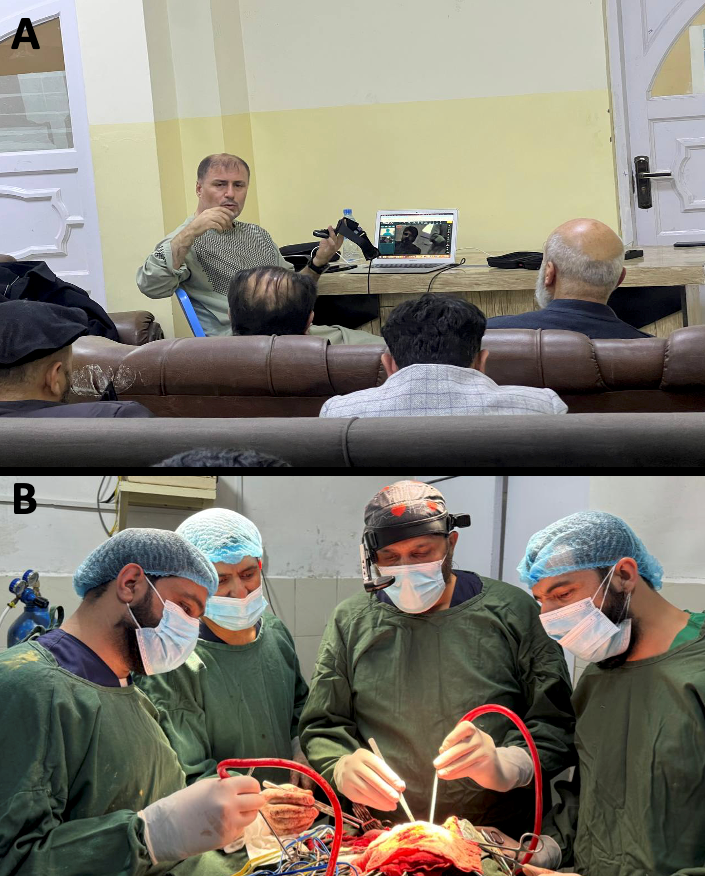
Figure 1: The “A” shows Dr. Jaweed, an Afghan neurosurgeon, providing training to fellow neurosurgeons in Afghanistan with Ohana One glasses. The “B” depicts Dr. Zamriduddin Khalid, a neurosurgeon based in Afghanistan, using Ohana One glasses during surgery.










