Bringing Polemic Issues with Inchoate Guidelines into Sharper Focus
Case Description
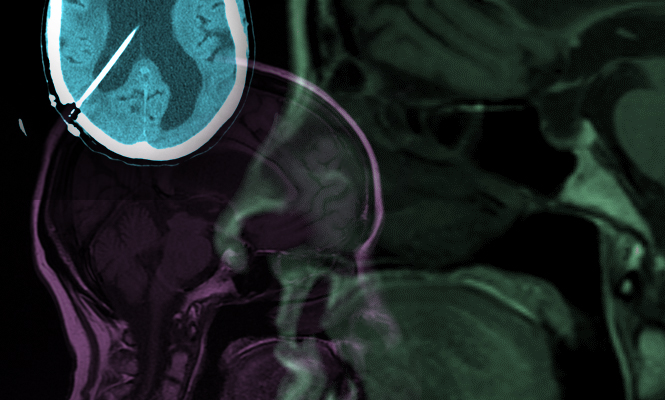
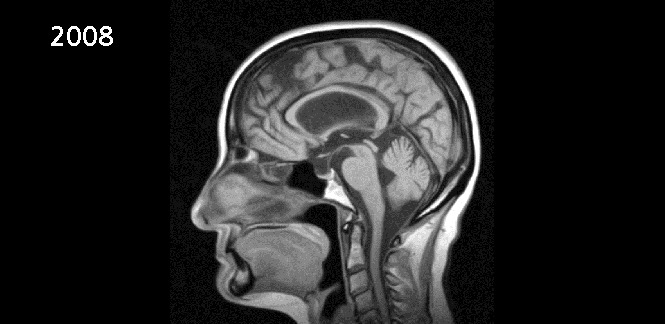
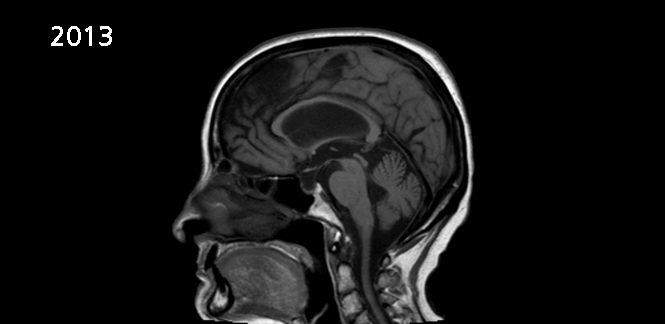
This 77-year-old, right-handed Caucasian woman presented with a two-year history of progressive unsteadiness, widening of her gait, urinary incontinence and short-term memory loss. She previously had an MRI in 2008 that showed hydrocephalus; reportedly, at that time, she did not have these symptoms. An MRI from 2013, when she saw us, showed slight increase in the size of the lateral and 3rd ventricles. The 4th ventricle size, by comparison, was not as large. Cortical atrophy was noted that was slightly more pronounced on the follow- up scan. There was no clear stenosis of the Aqueduct of Sylvius. Her neurological examination was normal except for a broad-based shuffling gait.
[aans_poll id=”1037″ view=”prompt”]
The Experts Weigh In
[aans_expert_comments title=”Marvin Bergsneider, MD, FAANS; Los Angeles”]
With patients with triventriculomegaly, we routinely obtain a sagittal CISS (Fast Imaging Employing Steady-state Acquisition, or FIESTA) MRI study to rule out an aqueductal web. If present, an endoscopic third ventriculostomy (ETV) would be offered. Otherwise, this patient would undergo an external lumbar drainage (ELD) trial to both assess if, and how much, she will improve with CSF drainage. The ELD study can also identify patients susceptible to over-drainage symptomatology. If she experiences a positive effect with the ELD trial, she would be offered a shunt procedure. Patients with truncal obesity, worrisome for peritoneal adhesions, are offered ventriculoatrial (VA) shunts, whereas all others are offered ventriculoperitoneal (VP) shunts. In our experience, lumbar-peritoneal (LP) shunts have a higher failure rate and are very difficult to manage with regard to the programmable valve.
Our experience with ETV for “communicating” NPH has been disappointing. Most experienced some mild temporary improvement, but nowhere near the degree of improvement they enjoyed with the ELD trial. All subsequently went on to shunt placement, signifying that ETV in this scenario had a poor risk-benefit ratio.
Continued observation would be a poor choice as well. This patient should have been evaluated for NPH in 2008. This disorder causes progressive brain damage. The idea of watchful waiting is a relic of an era when the risks of shunting elderly patients was unacceptably high. With the advent of programmable (adjustable) valves and prudent initial valve settings to avoid over-drainage, hydrocephalus should be addressed early in its course.
[/aans_expert_comments]
Discussion
Ventriculoperitoneal (VP) shunting with a programmable valve is the standard of care for symptomatic normal pressure hydrocephalus (NPH). The safety and effectiveness of the procedure has allowed it to supplant other options such as lumboperitoneal or ventriculoatrial shunting, although these are still considerations in select circumstances. It also is better than the natural history of the condition; NPH is a treatable cause of dementia and untreated patients progressively show a deterioration in all the cardinal symptoms and signs of NPH over time.
Over the past decade, there has been some discussion of the role of endoscopic third ventriculostomy (ETV) in the treatment of idiopathic NPH and secondary NPH (that follows head trauma, infection, or subarachnoid hemorrhage). There is some evidence that lends credence to this approach. It is known that imaging studies in NPH patients may demonstrate dilated lateral and third ventricles and thinning of the corpus callosum without concomitant dilatation of the fourth ventricle. The cause of this is not known and it is not considered prima facie evidence of aqueductal stenosis; on the other hand, although third ventricle enlargement is seen, it is not common to see the floor of the third ventricle thinned out and bulging downward as seen with classic aqueductal stenosis and obstructive hydrocephalus. Nonetheless, it does provide the opportunity to consider an ETV.
The access to the floor of the third ventricle is easy, with a wide open foramen of Monro, the pre-pontine cistern is usually capacious, and you avoid implanting a shunt with the associated risk of over-drainage. I have carefully selected a few patients with NPH over the years with this imaging finding of tri-ventricular hydrocephalus and a normal-sized fourth ventricle and given them the option of a VP shunt or ETV. In the few that elected to proceed with an ETV, my experience has been as follows; the procedure is simple and easy to perform, the complication rate is negligible with careful standard ETV technique (one caveat: the basilar apex may be enlarged and tortuous in these elderly patients. I always use a blunt probe to fenestrate the floor of the third ventricle and take care to stay anterior to the vessel), but the results have been modest. Patients do report an improvement in their symptoms but it is transient.
There are factors that may explain the lack of a lasting response to ETV in patients with NPH; the lack of elevated intraventricular pressures (the periventricular hypodensity seen in these patients is thought to be due to subcortical vascular encephalopathy rather than elevated intraventricular pressure), inadequate egress of CSF volume out of the ostomy in the floor of the third ventricle, and poor cerebral compliance. By contrast, VP shunting with programmable valves provides a robust CSF drainage pathway that can be regulated based on the patient’s symptoms and postoperative imaging findings, in order to provide an optimal level of drainage while minimizing the risk of complications, such as a subdural hematoma.
This is my practice: I use a lumbar drain trial when there is a doubt as to the cause of the patient’s symptoms, or when there are additional factors such as cognitive decline due to co-existent cerebrovascular dementia or other neurodegenerative conditions that may cloud the clinical picture. Patients with concordant imaging findings and clinical symptoms (even two of the three classical NPH triad, may suffice) are offered a VP shunt. I set the valve at 1.5 and then make further adjustments based on how the patient is doing and how the follow-up CT scans look. I reserve the option of an ETV in the rare instance when a shunt is precluded due to issues such as abdominal problems, medical co-morbidities or infection concerns. In the past, I have utilized the ETV option for selected patients with dilatation off the lateral and third ventricles out of proportion to the fourth ventricle, but my experience suggests that although this is a reasonable procedure, the long-term benefits are not as robust as seen with ventriculo peritoneal shunting. In the case described here, the patient’s symptoms improved after the ETV and then recurred a few months later. I placed a VP shunt with a programmable valve set at 1.5 and she has had a dramatic and lasting improvement in her symptoms without any new problems.
Results from previous Gray Matters Survey
Topic: Colloid Cyst
[aans_poll id=”1082″ view=”results”]
[aans_authors]
Suggested reading
1. Kiefer M, Unterberg A. The differential diagnosis and treatment of normal-pressure hydrocephalus. Dtsch Arztebl Int. 2012 Jan;109(1-2):15-25.
2. Torsnes L, Blåfjelldal V, Poulsen FR. Treatment and clinical outcome in patients with idiopathic normal pressure hydrocephalus–a systematic review. Dan Med J. 2014 Oct;61(10):A4911