A Letter from Medicare
On Nov. 5, 2018, the Centers for Medicare & Medicaid Services (CMS) Administrator, Seema Verma, issued a letter regarding evaluation and management (E/M) office visit coding. Specifically, Ms. Verma noted the fact that the coding scheme for E/M was developed in the 1990s and since that time the nature of clinical work in medicine has evolved into patient-centric collaborative models with clinical teams working in unison – a model that the 1990’s framework does not capture. Furthermore, Ms. Verma noted that a major cause of physician burnout is the documentation burdens associated with E/M coding. She stated that a change was long overdue.
Any neurosurgeon reading that correspondence would likely agree with many of its sentiments. After all, there is little to disagree with in those statements. E/M coding is indeed complex and out of proportion to the dollar value of the services provided. The code sets are out of date (1995 and 1997) and are becoming less congruent with the changing healthcare system. Many of us have found ourselves focusing on the technicalities of a particular code, which forces us into excessive documentation to justify the code selected and capture the value of our work. We all believe that that time would be better spent focusing on the patient.
Invoking the spirit of “Patient’s over Paperwork,” CMS has proposed a single payment rate for visits that are currently reported as levels two, three and four, which represent the majority of office visits. The documentation required for payment would be limited to what is currently required for a level two visit. A separate payment rate would remain for the most complex patients, those patients for whom a level 5, with the possibility of using time or medical decision making to justify the level of coding. The coding and reimbursement scheme would resemble Table 1 below.
In short, the five levels collapse into two for both new patients and established. Patient visits would either fall into routine or complex. Absent a new plan developed by organized medicine, the CMS proposal is slated to become effective on beginning on Jan. 1, 2021.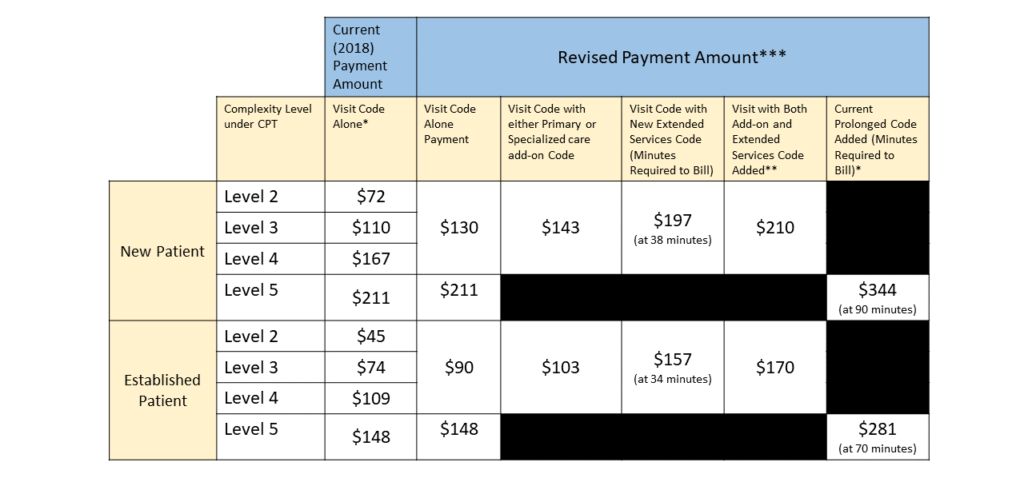
Table 1. The new proposal eliminates the level 1 code, and combines levels 2, 3 and 4 into one code for both new patients and established patients. Level 5 codes would require documentation with time, medical complexity or application of the previous criteria.
The Valuation Process of a CPT Code
The E/M codes represent the work product of the CPT Editorial Panel, a representative body from the American Medical Association (AMA). As such the AMA, the Congress of Neurological Surgeons (CNS) and the American Association of Neurological Surgeons (AANS) strongly objected to CMS proposing a new coding scheme outside the auspices of the AMA/Specialty Society Relative Value Scale (RVS) Update Committee (RUC). In response to the feedback from the various societies, CMS responded by saying,
“We (CMS) recognize that many commenters, including the AMA, the RUC, and specialties that participate as members in those committees, have stated intentions of the AMA and the CPT Editorial Panel to revisit coding for E/M office/outpatient services in the immediate future. We note that the 2-year delay in implementation will provide the opportunity for us to respond to the work done by the AMA and the CPT Editorial Panel, as well as other stakeholders. We will consider any changes that are made to CPT coding for E/M services, and recommendations regarding appropriate valuation of new or revised codes.”
The Chairs of the CPT Editorial Panel and American Medical Association (AMA)/ Specialty Society RVS Update Committee (RUC) created the CPT/RUC Workgroup on E/M Coding in order to solicit feedback on the best coding structure to decrease the burden of documentation while ensuring appropriate valuation. A code change application was submitted through the appropriate channels for consideration by the CPT Editorial Panel at the February 2019 meeting and passed.
In the new proposed CPT E/M code structure, it was determined that code level selection might be based either solely on medical decision making or total time on the date of the encounter. The extent of history and physical examination will no longer be an element in the code level selection of office visits. The new scenario deletes code 99201, as that code was not commonly used by physicians, but preserves codes 99202- 99295 and 99211-99215 and a creates a new prolonged visit add-on code 99XXX. The most important aspect of these new codes is that it represented the work product of a representative body from the AMA and national specialty societies. Fifty-two specialty societies have participated in the RUC surveys, among them were 1,000 randomly selected neurosurgeons. The survey asked questions about physician work and practice expense. At this writing, the surveys are completed, and data from those surveys were presented at the April 2019 RUC Meeting.
How will the new E/M coding scheme affect my practice?
The logical question we should ask is how these changes will affect our practice. The ultimate impact of the changes to E/M coding is difficult to assess. In the proposed 2019 Medicare Physician Fee Schedule (MPFS), CMS stated that the E/M changes would be minimal or possibly slightly positive for neurosurgery. However, in the 2019 Medicare Physician Fee Schedule (MPFS) final rule, CMS estimated that if they had implemented their E/M coding and reimbursement changes in 2019 rather than putting them off until 2021, the impact on neurosurgery would have been -1 percent in CY 2019. Further modeling by outside consultants estimates that the impact of these changes could result in an overall cut in overall Medicare payments to neurosurgeons by as much as 4 to 6 percent.
The impact of the CPT-approved/RUCvalued new codes will not be knowable until after the RUC meeting in April 2019 and will not be public until CMS publishes the information. It is important to recognize that even though a neurosurgical practice generates most of its revenue from surgical volume, E/M coding may represent upwards of 25 percent of the revenue.
Timeline: When will the new E/M coding scheme take effect?
There is little doubt that the new E/M office visit codes will be implemented by Jan. 1, 2021, in one form or another. Following the RUC action, CMS may provide some indication of the agency’s views when it releases the 2020 MPFS proposed rule sometime this summer. If the CMS states that it is inclined to accept the AMA CPT-passed/ RUC-valued codes and scuttle their original plan to collapse the codes, organized medicine would have another opportunity to provide public comments on a new plan.
The CNS and the AANS have been adamant in our insistence that should the E/M office visit values be increased, the E/M work built into the 10- and 90- day global surgical periods should be increased accordingly. Ideally, CMS would finalize the AMA CPT/RUC passed plan in the 2020 MPFS final rule released in November 2019. An implementation of Jan.1, 2021, will provide specialties a year to prepare and educate their members for the changes. Once CMS publishes comments about the RUC submission, it will be public information. The hope is that the new coding scheme will be the product of a representative body of physicians not a mandate from a government agency outside of the valuation process that has been established by organized medicine.
What should I do to prepare my practice?
It is important that neurosurgeons be aware of the impending changes for E/M coding. The coding software in the electronic medical record will need to be updated to include the new coding scheme, and ancillary coding staff and neurosurgeons will need to be trained on the new codes. When the new E/M office visit coding scheme is finalized, the Washington Office will provide educational information. Also, the AANS coding courses and CNS coding webinars will cover that material in great depth.
PLEASE NOTE, THIS IS PART ONE OF A PLANNED TWO ARTICLE SERIES ON THE SUBJECT OF THE NEW E/M OFFICE VISIT CODES.
A SECOND ARTICLE IS PLANNED TO PROVIDE ADDITIONAL GUIDANCE AND EDUCATION TO MEMBERS WHEN MORE INFORMATION IS MADE AVAILABLE BY CMS.
[aans_authors]








