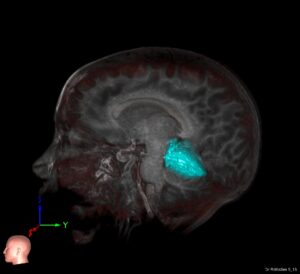
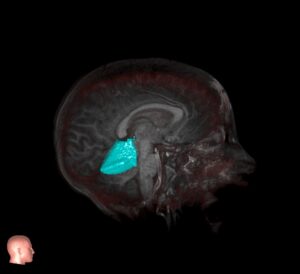
The patients have headaches and anxiety, the cranial imaging (and radiologist report) is scary –the referring doctors demand immediate action! The diagnosis can be nothing other than an arachnoid cyst. Every neurosurgeon has gotten the call and spent many hours with patients.
Understanding Arachnoid Cysts
Arachnoid cysts were first described in the 16th century, when a suprasellar arachnoid cyst was discovered at autopsy of a female with polyuria and blindness.1 With time, our understanding of these intracranial abnormalities has increased regarding:
- Composition
- Possible mechanisms of enlargement
- Etiology (largely congenital)
They are rare with an incidence of approximately 1.4% and a risk of enlargement around 2%.2 Best practice, however, remains intensely controversial. With the relative ease of access to information on the internet and recent high-profile cases of individuals with arachnoid cysts, neurosurgeons are now faced with debunking the perceived risks of these most often incidental findings. A quick Google© search of “arachnoid cyst” also suggests searches for:
- “… and anxiety”
- “… symptoms in adults”
- “Are arachnoid cysts fatal”
- “Is an arachnoid cyst dangerous”
Insight into the information readily available and popularly searched suggest that this diagnosis, though considered benign in our community, reveals a fearful reputation among the public. Even the medical literature thrives on reports of the unusual, with reports in the literature over several decades of arachnoid cysts associated with subdural hematomas – even as recent as 2018.3
Historical Help
Traditionally, intervention for arachnoid cysts was based on symptoms at presentation – most commonly headaches, which raised concerns of increased intracranial pressure. Other motivations for aggressive treatment included middle fossa arachnoid cysts thought to be the cause of associated seizures. This theory did not pan out in practice.4 The most common treatment was placement of a cysto-peritoneal shunt, both safe and radiologically effective (reducing the cyst volume), but with the real and devastating risk of causing shunt dependency.5,6 In certain circumstances, more invasive procedures, like craniotomies, were utilized to fenestrate large cysts. It was rare to involve a neurologist to manage headache or attempt to measure intracranial pressure via ophthalmologic exam or pressure monitor, as many of the interventions were based upon the relative mass effect upon the underlying brain, including signs such as sulcal effacement or scalloping of adjacent bone. A challenge in intervening upon these cysts has been in understanding their flow dynamics and whether fluid diversion or fenestration has a lasting effect. Unfortunately, symptom relief was unpredictable, and in some cases, the change in intracranial pressure dynamics created iatrogenic hydrocephalus, which has proven challenging to treat.
Treatment Reality vs. Patient Fears
Despite the increase in awareness of the general public and overall concern after an arachnoid cyst diagnosis, neurosurgery has begun to understand that these are often benign entities. Risk versus benefit analyses has increased the threshold for intervention.7 As our understanding of arachnoid cysts has evolved, and technology has advanced, our paradigm for treatment has become more conservative. In the words of the late Maya Angelou,
“I did then what I knew how to do. Now that I know better, I do better.”
Natural history studies have shown the low risk of change over time. Even evaluation of pediatric patient activities has given reassurance that these children may not be at any higher risk for severe intracranial injury with participation in contact sports.8 Yet, very selective arachnoid cysts may warrant intervention, specifically:
- Those causing accelerated head growth in younger patients.
- Cysts associated with significant midline shift.
- Cysts enlarging over time.
- Those causing obstructive hydrocephalus.
Higher resolution MRIs allow us to visualize the cyst walls with better definition and CINE flow studies can allow evaluation of CSF flow through the cyst. With improvements in endoscopic techniques and evolution of flexible endoscopy, minimally invasive options for fenestration are available for those arachnoid cysts requiring more invasive open surgery. Intraoperative navigation and virtual reality platforms allow for preoperative planning to reduce morbidity. Clearly, our better understanding of the long-term complications of shunt dependence makes this treatment a second option.
Ideally, as our understanding of the etiology of arachnoid cysts and impact upon the surrounding brain improves, we may be able to improve our approaches to intervention and patient outcomes.
References
[expand title=”View All”]
1. Kivelä, T., Pelkonen, R., Oja, M., & Heiskanen, O. (1998). Diabetes Insipidus and Blindness Caused by a Suprasellar Tumor. Jama, 279(1), 48.
2. Al-Holou, W. N., Terman, S., Kilburg, C., Garton, H. J., Muraszko, K. M., & Maher, C. O. (2013). Prevalence and natural history of arachnoid cysts in adults. Journal of Neurosurgery, 118(2), 222-231.
3. Wu, X., Li, G., Zhao, J., Zhu, X., Zhang, Y., & Hou, K. (2018). Arachnoid Cyst–Associated Chronic Subdural Hematoma: Report of 14 Cases and a Systematic Literature Review. World Neurosurgery, 109.
4. Koch, C. A., Voth, D., Kraemer, G., & Schwarz, M. (1995). Arachnoid cysts: Does surgery improve epileptic seizures and headaches? Neurosurgical Review, 18(3), 173-181.
5. Li, C., Yin, L., Jiang, T., Ma, Z., & Jia, G. (2013). Shunt dependency syndrome after cystoperitoneal shunting of arachnoid cysts. Childs Nervous System, 30(3), 471-476.
6. Zhang, B., Zhang, Y., & Ma, Z. (2012). Long-term results of cystoperitoneal shunt placement for the treatment of arachnoid cysts in children. Journal of Neurosurgery: Pediatrics, 10(4), 302-305.
7. Choi, J. W., Lee, J. Y., Phi, J. H., Kim, S., & Wang, K. (2014). Stricter indications are recommended for fenestration surgery in intracranial arachnoid cysts of children. Childs Nervous System, 31(1), 77-86.
8. Strahle, J., Selzer, B. J., Geh, N., Srinivasan, D., Strahle, M., Martinez-Sosa, M., . . . Maher, C. O. (2016). Sports participation with arachnoid cysts. Journal of Neurosurgery: Pediatrics, 17(4), 410-417. [/expand]
[aans_authors]