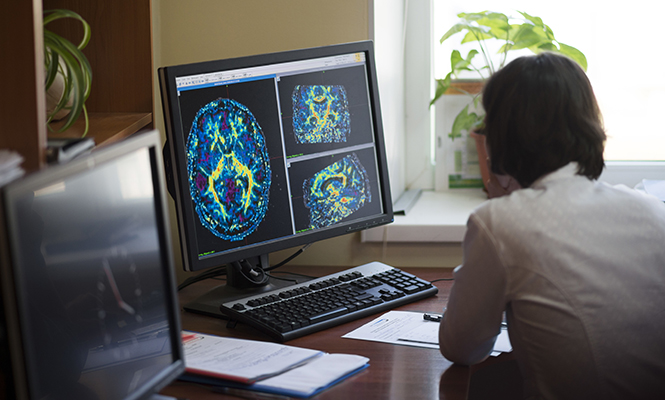
For many decades in neurosurgical history, even the diagnosis of low-grade gliomas (LGGs) was a challenge. Now, technological advances allow them to be readily diagnosed — sometimes in completely asymptomatic patients. This has led to dramatic swings in treatment recommendations. Early radical resections with many disastrous results led to an interval of simply biopsy or imaging surveillance. The pendulum has swung back.
Low Grade Gliomas
LGGs are uncommon lesions, accounting for about 15% of all gliomas, with a cumulative incidence of approximately 0.9 per 100,000 people.1 Contrary to the innocuousness suggested by their moniker, LGGs are malignant, infiltrative lesions that undergo a steady transformation into high-grade tumors over time. Surgical resection, radiation and chemotherapy allow us to improve upon the natural history of this disease to the benefit of our patients. But while many patients remain stable for years, the majority of patients with LGG will eventually succumb to malignant tumour progression.2
Heterogeneity: A Hallmark and a Challenge
The biological heterogeneity inherent in the diagnosis of LGG complicates attempts to define best practice for these patients and has likely tempered clinicians in their approach to treatment. With possible methodological flaws, even pre-MRI retrospective reports found a survival benefit with surgical resection for patients with LGG (five-year survival of 80-90%, versus 40-60% for biopsy). Subsequent studies in which extent of resection is determined by volumetric pre- and post-operative imaging demonstrate an incremental effect on both progression-free and overall survival.8 While compelling, these data suffer from many of the limitations inherent to retrospective surgical data. In addition, these data often leave authors unable to evaluate other important contributing factors due to insufficient information on variables, such as:
- Molecular sub classification;
- Systemic therapy;
- Histologic grade; and
- Hormone receptor status.
Our understanding of the role of surgery in low-grade glioma may be limited by analogous biases.
 These limitations have been circumvented by work from Jakola and colleagues. The authors took advantage of a unique situation in which two geographically close Norwegian hospitals have different treatment philosophies for patients with presumed LGG: one, biopsy followed by a wait-and-watch approach, and the other, an approach based on early resection. Assuming that the clinical features of the patients seen at hospital A would be comparable to the features of patients seen at hospital B as the two populations differ only in terms of home address, this dichotomy allowed the study of population-based parallel cohorts, in which the treatment strategy employed was highly dependent on the patient’s residential address. Jakola et al. found that, at the hospital favoring early resection, patients had marked improvement in survival compared with the patients treated at the hospital favoring biopsy and wait-and-watch: 80% vs. 70% survival at three years, and 68% vs. 44% survival at seven years. For patients with a Grade II astrocytoma, overall survival was 9.7 years at the center favoring early resection compared to 5.6 years at the center favoring biopsy. Time to malignant transformation, as determined by the finding of new enhancement on imaging, was shorter in the biopsy-only treatment group, suggesting an etiology for the longer overall survival seen in the group undergoing early resection.
These limitations have been circumvented by work from Jakola and colleagues. The authors took advantage of a unique situation in which two geographically close Norwegian hospitals have different treatment philosophies for patients with presumed LGG: one, biopsy followed by a wait-and-watch approach, and the other, an approach based on early resection. Assuming that the clinical features of the patients seen at hospital A would be comparable to the features of patients seen at hospital B as the two populations differ only in terms of home address, this dichotomy allowed the study of population-based parallel cohorts, in which the treatment strategy employed was highly dependent on the patient’s residential address. Jakola et al. found that, at the hospital favoring early resection, patients had marked improvement in survival compared with the patients treated at the hospital favoring biopsy and wait-and-watch: 80% vs. 70% survival at three years, and 68% vs. 44% survival at seven years. For patients with a Grade II astrocytoma, overall survival was 9.7 years at the center favoring early resection compared to 5.6 years at the center favoring biopsy. Time to malignant transformation, as determined by the finding of new enhancement on imaging, was shorter in the biopsy-only treatment group, suggesting an etiology for the longer overall survival seen in the group undergoing early resection.
Their study does not escape all limitations. As their analysis is retrospective, the authors cannot exclude the risks of crossover and reporting bias. In addition, the 95% confidence intervals of the two patient cohorts overlap—further follow-up will be necessary to determine that their conclusions are not the effect of chance. Finally, there was a slight preponderance of patients with oligodendroglioma in the resection group compared to the biopsy group (19% vs. 9%), though the author’s post-hoc findings that the effect of surgery was most pronounced in patients with astrocytic tumors seems to minimize the relevance of this discrepancy.
Interestingly, Jakola and colleagues found no significant difference in surgical morbidity between the patient cohorts treated with resection and biopsy. Multiple groups have shown that extensive preoperative planning and intraoperative functional mapping can allow surgeons to perform these procedures safely and effectively. For example, in a retrospective series of 100 patients with LGG who were operated on without intraoperative mapping and a series of 122 later patients who were operated on with concurrent use of electrocortical stimulation for brain mapping, Duffau and colleagues find that patients who underwent awake surgery with intraoperative mapping had a significantly lower rate of severe permanent deficits (6.5% vs. 17%), while benefiting from a higher rate of gross total resection (GTR) and subtotal resection (25% and 51% vs. 6% and 37%, respectively) and a survival advantage, compared to the initial group.10 Further, the authors found that the definition of a surgically accessible tumour increased significantly with intraoperative mapping.
These data have led to recommending surgery for patients with LGG, with particular emphasis on immediate intervention in patients harboring risk factors for early progression. Preoperative functional MRI and awake craniotomy have been employed with intraoperative functional mapping to reduce the risk of deficit associated with aggressive surgery and improve extent of resection.11 As radiotherapy has been found to lengthen progression-free, but not overall survival in this cohort12, radiation is reserved in patients who have undergone gross-total or near-gross total resection and for patients with high-risk disease.
References
[expand title=”View All”]
1. Porter, K. R., Mccarthy, B. J., Freels, S., Kim, Y., & Davis, F. G. (2010). Prevalence estimates for primary brain tumors in the United States by age, gender, behavior, and histology. Neuro-Oncology, 12(6), 520-527.
2. Shaw, E. G., & Wisoff, J. H. (2003). Prospective clinical trials of intracranial low-grade glioma in adultsand children. Neuro-Oncology, 5(3), 153-160.
3. Klein, M., Taphoorn, M. J., Heimans, J. J., Ploeg, H. M., Vandertop, W. P., Smit, E. F., . . . Aaronson, N. K. (2001). Neurobehavioral Status and Health-Related Quality of Life in Newly Diagnosed High-Grade Glioma Patients. Journal of Clinical Oncology, 19(20), 4037-4047.
4. Klein, M., Heimans, J.J., Aaronson, N.K., Postma, T.J., Muller, M., van der Ploeg, H.M. & Taphoorn, M.J. (2004). [Impaired cognitive functioning in low-grade glioma patients: relationship to tumor localisation, radiotherapy and the use of anticonvulsants]. Nederlands tijdschrift voor geneeskunde. 148(44), 2175-80.
5. Chang, E. F., Zada, G., Kim, S., Lamborn, K. R., Quinones-Hinojosa, A., Tyrrell, J. B., . . . Kunwar, S. (2008). Long-term recurrence and mortality after surgery and adjuvant radiotherapy for nonfunctional pituitary adenomas. Journal of Neurosurgery, 108(4), 736-745.
6. Veeravagu, A., Jiang, B., Ludwig, C., Chang, S. D., Black, K. L., & Patil, C. G. (2013). Biopsy versus resection for the management of low-grade gliomas. Cochrane Database of Systematic Reviews.
7. Pouratian, N., Asthagiri, A., Jagannathan, J., Shaffrey, M. E., & Schiff, D. (2007). Surgery Insight: The role of surgery in the management of low-grade gliomas. Nature Clinical Practice Neurology, 3(11), 628-639.
8. Smith, J. S., Chang, E. F., Lamborn, K. R., Chang, S. M., Prados, M. D., Cha, S., . . . Berger, M. S. (2008). Role of Extent of Resection in the Long-Term Outcome of Low-Grade Hemispheric Gliomas. Journal of Clinical Oncology, 26(8), 1338-1345.
9. Falk, L., Wright, J., Wolfe, L., & Deinhardt, F. (1974). Herpesvirus ateles: Transformation in vitro of marmoset splenic lymphocytes. International Journal of Cancer, 14(2), 244-251.
10. Duffau, H. (2005). Contribution of intraoperative electrical stimulations in surgery of low grade gliomas: A comparative study between two series without (1985-96) and with (1996-2003) functional mapping in the same institution. Journal of Neurology, Neurosurgery & Psychiatry, 76(6), 845-851.
11. Chang, E. F., Zada, G., Kim, S., Lamborn, K. R., Quinones-Hinojosa, A., Tyrrell, J. B., . . . Kunwar, S. (2008). Long-term recurrence and mortality after surgery and adjuvant radiotherapy for nonfunctional pituitary adenomas. Journal of Neurosurgery, 108(4), 736-745.
12. Bent, M. V., Afra, D., Witte, O. D., Hassel, M. B., Schraub, S., Hoang-Xuan, K., . . . Karim, A. (2005). Long-term efficacy of early versus delayed radiotherapy for low-grade astrocytoma and oligodendroglioma in adults: The EORTC 22845 randomised trial. The Lancet, 366(9490), 985-990. [/expand]