According to recent statistics, just 30 percent of Americans in the workplace are engaged — meaning they like who they work for, they like what they do and they feel fulfilled by their job. This low figure should provide pause for leaders because employees who are not engaged are unlikely to invest much effort for their employer. This holds true whether you are referring to a Fortune 500 company or a provider of health care.
Our recent experience in the neurosurgery clinic at University of Utah Health Care (UUHC) offers an example of how employee engagement can substantially impact metrics that are increasingly being used to measure the “value” of a health-care provider. As we move towards a pay for performance environment, we need clarity on how many factors, external to the provider him/herself, play a role in the patient’s perception on his/her episode of care.
Declining Exceptional Patient Experience Scores
To gauge what kind of experience the patients have in clinic, UUHC has partnered with Press Ganey Performance Solutions to send out patient surveys. The survey, which asks the patient questions regarding their experience with the staff and provider, is sent after each visit to all patients who provide email addresses. The survey is scored, analyzed and assigned a national percentile ranking that provides a comparison with other health-care organizations. Each year, every clinic at UUHC is assigned an Exceptional Patient Experience or “EPE,” an overall percentile based on national rankings. Additionally, weekly and monthly rankings are sent to the departments demonstrating the overall clinic scores as well as individual provider’s scores. Although some of the survey questions ask the patient to rate the staff and cleanliness of the clinic, the scores received are all tied directly to the care provider.
After several years of achieving scores in the 95th percentile or better, the first half of 2014 saw a precipitous decline in EPE Scores in the neurosurgery clinic, missing the predetermined national ranking goal by a substantial amount. These scores, reportedly reflective of the ambulatory patient-doctor interaction, changed despite no addition or subtraction of faculty members, alteration in provider schedules or change in care patterns. The only recognizable change was in administrative clinic leadership and staff.
In the midst of this downswing, the hospital and clinics were working on evaluating and improving staff engagement. This process included the creation of a new human resource support group for organizational development, which was available to any struggling clinics. In the first of many surveys done, clinic employees were asked to rate their level of engagement on several parameters, including citizenship, coworker relations, employee respect, growth and development, leadership, organizational alignment and work-life balance. We received the results of this first survey in late spring of 2014 and recognized that not only did we need to engage this new support group, but that this was the likely explanation for the plummeting scores.
Identifying Key Issues Affecting Staff Engagement
In August 2014, Emily Chipman from the organizational development group began a series of meetings with the neurosurgery staff to solicit feedback. Emily began the first meeting using a technique called “appreciative inquiry.” This technique solicits ideas from staff members on how to improve engagement in the office — relying on their own strengths to get them accomplished. In meetings without management present, the neurosurgery clinic staff provided dozens of ideas about what they wanted to see improved. After several meetings, the ideas were compiled, categorized by type of change and represented to the staff to vote on their top-five items to be improved. The top-five items on the list were indicative of issues that often affect work units: communication, accountability, team dynamics, staff education and reporting (how patient scores were reported to the staff).
Once the key issues affecting staff engagement were identified, each item was assigned a delegate within the staff to ensure changes were handled in a way that the staff felt would be valuable. As a team, the group decided how they wanted things moving forward, and the delegate would ensure they were followed through:
Communication — Meeting structure would be changed to ensure important items would be discussed often, and as an entire team.
Accountability — Clinic supervisors wished to create their own version of the daily duties list and have the ability to hold their team accountable to those duties.
Team Dynamics — The staff felt it was vital to add a requirement to the new daily duties list to check with your teammates often to see if they required assistance.
Staff Education — Once per month, meeting early in the day and all together as a clinic staff, guest speakers would visit the clinic and provide an in-service regarding their own specialty.
Reporting — Clinic staff wanted to hear more patient comments, and the numbers that followed.
The Results
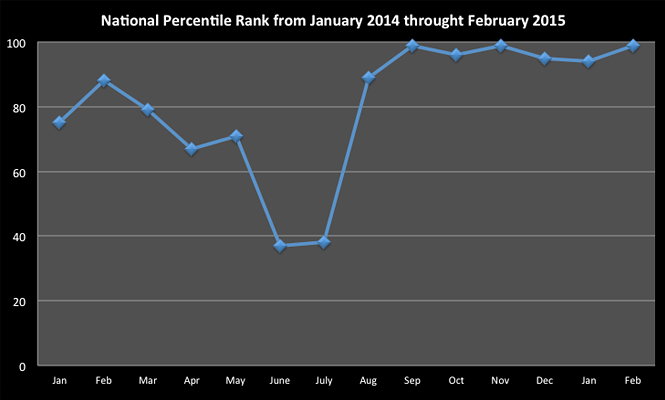
In the several months that followed, staff appeared more engaged, more satisfied with their work and happier with their team. Overall, the clinic’s staff reported feeling more valued and more involved in decisions, with a greater investment in the organization. Underscoring the perception of improvement was the change in the patient satisfaction scores. The results have been astonishing. In July 2014, mean scores on patient surveys had dropped below 90, which fell to the 38th percentile nationally. Within seven months, by February 2015, the mean scores increased to nearly 95, which boosted the neurosurgery clinic to the 99th-percentile nationally (Figure 1).
Without any other changes in the clinic procedures that directly affected patient care, the improvements in staff engagement had been recognized by the patients. The meetings soliciting feedback from the staff and the subsequent changes in the workplace had a dramatic effect on the patient experience, improving their opinions of the provider and the organization.
In a clinical health-care setting, the degree to which staff is engaged affects patients’ experiences, outlook on health care and overall impression of their provider(s). Thus, disengaged employees may have a disproportionate effect on a patient’s choice of health-care provider, and ultimately (and unfortunately) the provider’s practice and compensation.
It continues to challenge us as health-care providers to ensure that we not only are providing the optimal care for our patients, but also are responsible for each overall episode of patient care. As many of these relevant influences may be extrinsic to the physician, it is with great caution that we should interpret the results of these surveys. Additionally, it is imperative that we understand the role of these influences and how to manage or alter them in this age of “value-based” care that emphasizes measures — such as patient-satisfaction scores — as surrogate markers of quality-of-care.
[aans_authors]