
Overlapping surgery, also referred to as simultaneous surgery, concurrent surgery or “running two rooms,” is not uncommon in neurosurgery where caseloads are heavy and cases are long and there is much wasted time during anesthesia preparations and turn-overs between cases. Overlapping surgery has recently come under intense scrutiny following a Boston Globe Spotlight Team report examining this practice at Massachusetts General Hospital (MGH). Controversy was inflamed by this report because it suggested that patients were uninformed that they were sharing their surgeon with another patient, and that there might be increased complication risks as a result.
Where Do We Stand?
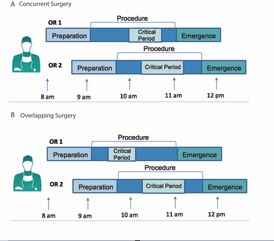
The American College of Surgeons (ACS), as well as the main neurosurgical societies (the AANS, Congress of Neurological Surgeons (CNS), American Board of Neurological Surgeons (ABNS) and the Society of Neurological Surgeons (SNS)), issued a position statement defining concurrent and overlapping surgery. “Overlapping surgery” was defined as two cases performed by one surgeon in different operating rooms with overlapping procedure times, but not an overlapping critical period. In contrast, “concurrent surgery” was defined as two cases performed by one surgeon in different operating rooms with overlapping critical periods. This group of neurosurgical societies also issued guidelines stating that “a primary attending neurosurgeon’s involvement in concurrent or simultaneous surgeries on two different patients in two different rooms is not appropriate,” whereas overlapping surgery was appropriate when the cases were staggered to keep critical periods of the cases from overlapping, a back-up attending neurosurgeon was immediately available if needed and the patient was informed of these circumstances.
A Look at the Numbers
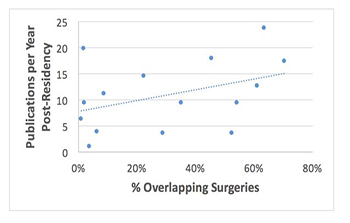
When the Senate Finance Committee asked for data from 20 academic medical centers about the safety of concurrent surgery, the University of California San Francisco was among those queried, and I was asked to participate in drafting a response. Reports were limited to a quality review of morbidity and mortality at MGH released on a website and an abstract from the University of Virginia examining operative duration, morbidity and mortality in coronary artery bypass surgery and valve replacements. Having practiced overlapping surgery for years and not noticed any safety issues, I offered up my results, specifically comparing outcomes from non-overlapping cases performed on a day of the week when I have a single block of OR time with outcomes from overlapping cases performed on two days of the week when I have two blocks of OR time.
We first analyzed 1,219 overlapping versus non-overlapping vascular neurosurgeries (1) and found that overlapping surgeries had longer procedure times (30 minutes) and more unplanned 30-day readmissions, but shorter hospital stays, higher rates of discharge to home, lower 30-day mortality rates, lower rates of acute respiratory failure and decreased 30-day unplanned returns to OR (1). Rates of severe sepsis, postoperative stroke, intraoperative aneurysm rupture and postoperative aneurysm residual were also equivalent between the overlapping and non-overlapping surgery groups (1). We then broadened the analysis to include nine neurosurgeons who perform overlapping surgery for all types of neurosurgical procedures (2), including spinal procedures (3), at our institution. Once again, we found similar results, with longer procedure times but similar patient outcomes in 3,752 overlapping as compared to 3,633 non-overlapping cases.
Taken together, this work is among the first to show that “running two rooms” can be done safely in the academic neurosurgery setting and the general public’s concerns can be answered scientifically with data. However, this work highlights the need for careful patient selection and case pairings, assistance from residents and fellows, attending-level back-up and patient awareness through informed consent. Overlapping surgery should only be performed with two operating rooms, not more. If a complex case is performed in a second room, it must be paired with a simple case in the first room. Two overlapping complex cases with long critical periods are more likely to become two concurrent complex cases. The attending should define the critical portion of the case for the entire operating team before starting the case, typically during the “time out,” and be present for that portion. The resident or fellow assisting in the surgery must have the appropriate training and skills to operate independently. A back-up attending neurosurgeon must be designated and available within minutes if needed.
Involve the Patient
Neurosurgeons who perform overlapping surgeries should be audited periodically to review outcomes and to ensure safe practices. Most importantly, the patient must be informed of the overlapping nature of the surgery and have given informed consent. Many neurosurgeons find this conversation with patients to be the most difficult part of the process. I typically bring it up after the decision to proceed with surgery has been made when we are discussing scheduling, at which time I explain that on the day we have selected, I run two rooms and will be splitting my time. If they are uncomfortable, I reschedule to a different day when I only run only one room. This discussion makes them aware of the practice and gives them the opportunity to opt out.
But what is the definition of the “critical period” of a case? Is it the aneurysm clipping, the dissection of the aneurysm leading to its clipping or the craniotomy, during which a mistake could lead to aneurysm rupture or critical bleeding? The “critical period” is vague and varies from case to case but should be individualized by the attending surgeon who understands the interrelationships between the patient, the pathology, the team and the day’s circumstances. Outside administrators and regulators will try, or are actively trying, to define this critical period of an operation for neurosurgeons, and they might resort to tracking devices, punch clocks or video surveillance to enforce two-room policies. We must accept the responsibility of defining and covering the critical portions of the case, if we hope to defend and retain the privilege of running two rooms.
Why is overlapping surgery so important for us to support collectively when the public might perceive it negatively? Overlapping surgery allows neurosurgeons to treat patients in a more timely manner, decreasing wait times and backlogs, thereby increasing access to specialized neurosurgeons. Overlapping surgery might increase the safety of our procedures by performing them during daylight hours with rested and optimized teams, rather than late at night with tired and inexperienced teams. Overlapping surgery improves efficiency and quality of the neurosurgeon’s life, shortening the day and guarding against burnout and frustration. Perhaps most importantly, overlapping surgery increases surgical volume, which translates to experience, technical expertise and superior outcomes. The association between high-case volume and improved patient outcomes is well-established (4,5), and famously busy cardiac surgeons like Michael Ellis DeBakey, MD, and Denton Cooley, MD, demonstrate how vast experience can lead to surgical advances and pioneering work.
Another important byproduct of overlapping surgery is that it creates unique learning opportunities for residents and fellows. Trainees learn through observation, observed operation and unobserved operation. With the first method, the resident observes and assists the instructor, who then safely and quickly completes the surgery. With the second method, the instructor observes and coaches the resident, which may slow the surgery but still ensures safety and educational value. With the third method, the resident operates independently, which is a coveted learning opportunity for him or her, while the instructor works in a second room and maximizes productivity. Autonomy is critical in training the next generation of young neurosurgeons to develop their manual dexterity, make intraoperative decisions on their own and confront pathology firsthand. Learning requires a combination of these three methods, and overlapping surgery fosters this.
While considerable debate still rages publicly and in Congress about concurrent surgery and the final outcome is uncertain, it is important to examine hard data. Our outcomes suggest that “running two rooms” can be done safely with careful patient selection, case pairings, resident/fellow assistance, attending back-up and patient awareness. Increased surgical volume leads to technical expertise and superior outcomes, which are the ultimate prizes that neurosurgeons seek. Overlapping surgery, therefore, is an essential element in the pursuit of mastery, beginning in residency training and continuing throughout our careers.
[aans_authors]





