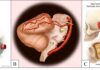
Jessica Gebhardt was 31-years-old in May 2014 when she was the driver in a motor vehicle accident (car versus tree) resulting in polytrauma. Her Glasgow Coma Scale grade was six upon EMS arrival at the scene. After prolonged extrication, she was intubated on the scene and transported via helicopter to the University of Toledo Medical Center (Level One Trauma Center). Her initial head CT scan showed thin bilateral subdural hematomas (R>L) and contusions (bilateral frontal lobes R>L and right temporal lobe). She had multimodal invasive-brain monitoring (ICP via ventriculostomy and brain tissue oxygenation) and was managed with aggressive medical therapy until her intracranial pressure became recalcitrant to further medical management, and ultimately, underwent a right-sided decompressive craniectomy. She emerged from coma about three to four weeks after the initial injury and has made exceptional progress since. The accompanying story is written by the patient and her husband explaining their experience with neurosurgical care for severe traumatic brain injury.
-Jason L. Schroeder, MD, FAANS
By Josh Gebhardt
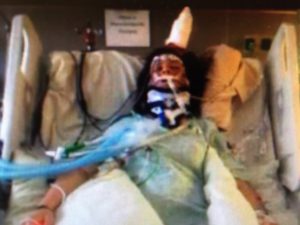
On May 25, 2014, my wife and I were in a car accident. She suffered a shattered right patella with a partially-torn left quadriceps tendon, in addition to a contusion on the right frontal lobe of her brain. She laid in a medically-induced coma for approximately four weeks and underwent surgeries to repair both knees, as well as a craniotomy to remove the right bone flap of her skull. Her traumatic brain injury (TBI) eventually led to seizures and a series of strokes in the left hemisphere of her brain before she was brought back to consciousness. She cannot yet write, so she asked me to provide this perspective of the events based on both my experience and what she remembers.
 A Whirlwind of Fear and Confusion
A Whirlwind of Fear and Confusion
It started with a crash. The minutes and hours that followed are probably the stereotypical description from anybody who’s just been in an automobile accident; a hazy whirlwind of fear, confusion and adrenaline. I remember having no idea how badly my wife was hurt. As I lay strapped to my own stretcher in a lonely ER room, waiting to see the doctor for what seemed like forever, I was anxious to speak with her, and was expecting the staff to tell me my wife had just come out of surgery to repair her broken leg (which was visibly obvious at the scene), and that she would be just fine.
When Dr. Schroeder entered and explained to me the extent of my wife’s injuries, I was — as you might expect — in total shock; but even then, I had no grasp on what everything I was just told actually meant. Over the next 48 hours, it became clear to me we wouldn’t be going home anytime soon. Myself, along with friends and family, set up camp in the ICU waiting room and I remember not being able to fully process the situation. Don’t misunderstand me, I could interpret what the doctor said, and I could see Jessica laying in the bed, but it didn’t feel like reality. There was a conflict between what my eyes perceived, and knew to be true, with what felt real. As I went through each day living in this new setting, my mind eventually accepted it.
Jess’ recollection of things didn’t begin until about 30-odd days after mine. She can recall bits and pieces of her stay in the ICU, such as some nurses and visitors, but she doesn’t have a fluent memory of her time there. She told me that she only thought her knees were banged up. When we arrived at Dodd Hall, at The Ohio State University Medical Wexner Center, to start intensive inpatient therapy, she was angry. She remembers thinking that the ambulance transport was taking her home, so the reasons for her frustration and disappointment are now obvious. As she recalls, even several weeks into therapy, she had no idea she suffered a TBI. In her mind, she was just trying to heal her knees. It wasn’t until she had her bone flap replaced that she began to understand she had a head injury. I’ve come to believe that God shielded her from that realization in order to protect her from the emotional turmoil it was sure to bring. Our time at Dodd was amazingly productive. Jess progressed, and we were sent home almost three months to the date after the accident.
Returning Home
From my perspective, that was the most difficult and stressful time. Jess was so fragile, and suddenly, I didn’t have a full-hospital staff ready to come to my aid when I had a question or concern. Home felt so foreign, compared to what it was, when we left for what we thought would be a long weekend. I was terrified with every decision I made. Did I let the visitors stay too long? Should I have had visitors come? Was she eating enough? It was overwhelming to feel like her recovery hinged on how well I was able to care for her.
Jess remembers being glad to be home, and was still unaware at that time of how fragile she was. The most difficult time for Jess came about two months after our homecoming. The initial swarm of visitors had slowed down, and everybody’s schedule, including ours, became bogged down with the hustle and bustle of the holidays. Compounding the problem, was the fact Jess’ phone had broke. Due to the fact she couldn’t really read or write at the time, I thought little of it. However, as she healed, she told me how cut-off and depressed it made her feel by not having it. Her emotional state declined without it, and then improved dramatically once it was replaced.
 After completing physical therapy, we began attending the local YMCA. Jess has always loved running, but because her knee still lacked flexion, and due to the fact she was still so skinny, I encouraged her to lift weights in hopes she would pack on some mass. This turned out to be a huge factor in her recovery. Jess’ knee improved, and her strength and balance progressed; she became even more driven and happy. Jess has told me that finding her way to the weight room has been a hugely positive factor in her recovery.
After completing physical therapy, we began attending the local YMCA. Jess has always loved running, but because her knee still lacked flexion, and due to the fact she was still so skinny, I encouraged her to lift weights in hopes she would pack on some mass. This turned out to be a huge factor in her recovery. Jess’ knee improved, and her strength and balance progressed; she became even more driven and happy. Jess has told me that finding her way to the weight room has been a hugely positive factor in her recovery.
Relying on Faith, Not Fear
Another large factor aiding her recovery was the eagerness of her employer to welcome her back to work. Jess is a surgical nurse and passionate about her profession. Though she wasn’t able to perform her duties yet, her administrator allowed her to hang around the OR to re-familiarize herself with the setting and spend time with the close-knit staff. As time went on, and she continued to heal, they began easing her back into her duties. She now works three days a week as a surgical tech and continues to inch toward her ultimate goal of returning as a full-time RN.
Without question, the biggest and most important factor in all of this has been God. We’ve felt his hand on us this entire time, and the option to rest in our faith rather than dwelling in fear has kept us going. We have no doubt that we were guided into the care of Dr. Schroeder, who we are forever indebted to, and whose skill and talent are evident by Jess’ recovery. We also know that God put out an SOS call for us that was answered by more people than we could ever be worthy of being helped by. We were blessed with loving and skilled therapists and provided for in every way. We give God all the glory for his power, love, faithfulness and we give our deepest thanks to all those who helped us along the way.
 Jess continues to progress each day. Little by little, her speech improves and her ability to read returns. She drives, works, and hangs out with friends. As her awareness progresses, she is learning to cope with the frustration of dealing with the lingering side-effects of the injury, but we will continue to be patient, as we know God has placed us in good hands and that he won’t stop carrying us now.
Jess continues to progress each day. Little by little, her speech improves and her ability to read returns. She drives, works, and hangs out with friends. As her awareness progresses, she is learning to cope with the frustration of dealing with the lingering side-effects of the injury, but we will continue to be patient, as we know God has placed us in good hands and that he won’t stop carrying us now.
Jessica Gebhardt, a surgical nurse from a small town in Ohio, is known for being both hard-working and sweet. Her friends are co-workers describe her as “everybody’s favorite.” Josh Gebhardt, also from a small town, is a sworn deputy and works full-time as a juvenile probation officer. [aans_authors]