Parents, physicians and the general public have increasingly expressed concerns about traumatic brain injury (TBI) and concussion in youth contact sports. The decrease in youth sports participation could be a reflection of this issue.2 Youth sports participation decreased by almost 10 percent between 2009-2014.3 These concerns are legitimate and based on the well-known risks of sports-related TBIs among youths. The incidence of sports-related concussion (SRC) among high school athletes during academic years 2011-2014 was almost four, per 10,000 athletes, per game.1 The highest risk was seen with:
- Boys’ football: 9.2 per 10,000
- Girls’ soccer: 6.1 per 10,000
Conversely, medical benefits for both youth contact and non-contact sports include decreased risks of hypertension, obesity,4 diabetes,5 cardiovascular disease, dementia, osteoporosis and thirteen types of cancer.6
Support for Limiting Youth Contact Sports
This conundrum has led to conflicting attitudes about youth contact sports. Overwhelmingly (81 percent), pediatricians support limiting or eliminating tackling in youth American football.8 Do physicians of other specialties, who often treat head injuries and sports trauma, hold similar perspectives? An electronic survey investigated the opinions of 74 neurosurgery and 107 orthopedic surgery department chairs regarding bans and limitations in youth, collegiate and professional contact sports (Table 1).
Survey response was sufficient, with 43 percent orthopedic chairs and 61 percent neurosurgery chairs reporting and generating interesting results. Increased age led to less  support in both specialties for limits or bans on:
support in both specialties for limits or bans on:
- Boxing
- Head-hitting in martial arts
- Tackling in football
- Heading in soccer
- Body-checking in ice hockey
- Off-piste skiing or snowboarding (Figure 1)
Neurosurgeons Support Greater Limitations
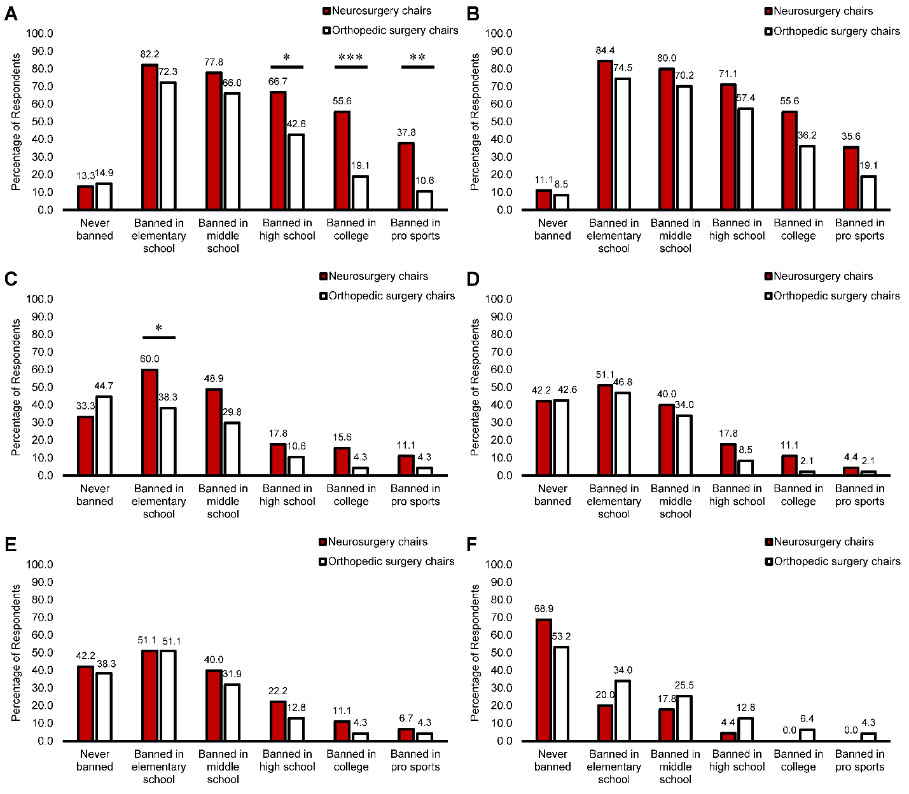
Both cohorts of respondents showed greatest support for bans on head-hitting in martial arts and the entire sport of boxing at all age groups. Bans on off-piste skiing or snowboarding had the lowest support. Key findings include:
- The majority of chairs supported banning the entire sport of boxing for elementary and middle school youths.
- More neurosurgery chairs supported banning the entire sport of boxing for high school (X2 = 5.388, p = 0.020), collegiate (X2 = 13.078, p < 0.001) and professional groups (X2 = 9.306, p = 0.002).
- More neurosurgery chairs supported implementing a ban on tackling in football for elementary school youths (X2 = 4.333, p = 0.037), relative to orthopedic chairs.
- There was equivalent and less support for banning football tackling in older youth, collegiate and professional groups.
- Orthopedic and neurosurgery chairs had comparable opinions about all other contact sport types in every age group. (Figure 1)
In probable contrast to historic opinions, recent data about the impact of TBI and youths has led the majority of both orthopedic and neurosurgery department chairs to support limitations on contact sports, especially in the youngest age groups. Neurosurgery chairs seem to have more conservative viewpoints on boxing and youth football.
Speculating on Differential Attitudes
Requirements for board certification9 and training requirements set by the ACGME in neurosurgery and orthopedic surgery include critical care in trauma with dedicated trauma exposure.10,11 Neurosurgeons, however, have more exposure to TBI care and management, as 8.8 percent of all TBI cases require neurosurgical intervention.12 Thirty-two percent of brain deaths under the care of neurointensivists and neurosurgeons are due to TBI.13,14 Nevertheless, there has been increasing emphasis for orthopedic surgeons to acquire experience in TBI diagnosis and care.15
Toward an Integrated Approach
In addition to the acute care provided by orthopedics and neurosurgery for trauma, other specialists are integrally involved in chronic and long-term care, such as pediatrics, neurology and sports medicine. Physicians across these specialties comprise a team responsible for acute and chronic management of youth trauma and TBI and consolidation of their opinions on the risks and benefits of contact sports is necessary for better care of youth athletes. Because physicians are also educators about these medical issues, a more integrated set of perspectives on youth contact sports will more effectively inform the public.
No Easy Answers
The risks and benefits of youth contact sports ultimately have to be weighed against the benefits of non-contact sports, which may be safer alternatives that can provide similar benefits of a physically active lifestyle. However, the risks of contact sports relative to non-contact sports are not obvious. A cohort study of 3,794 youth athletes (grades 2-7) shows that the hazard ratio of injury from flag football was 2.22 times higher than that of tackle football.16 The comparative hazard ratio of flag football and tackle football was not significant for severe injuries (0.949) or concussions (1.96),16 suggesting that the contact nature of a sport does not necessarily indicate a higher risk of injury. Likewise, men’s and women’s hockey have nearly equivalent concussion rates, despite the fact that body-checking is allowed only in men’s hockey.17 Further research and continuing medical education for all physicians involved in the management of youth and adult TBIs and trauma will be necessary to better understand the complex nature of the risks and benefits of contact sports.
Table 1. Survey question sent to neurosurgery and orthopedic surgery department chairs. All of the Responses are available for each sport.
Figure 1. Differences between neurosurgery (N = 45) and orthopedic surgery department chairs (N = 47) in opinions on implementing bans against (A) boxing, (B) head-hitting in martial arts, (C) tackling in football, (D) heading in soccer, (E) body-checking in hockey and (F) off-piste skiing or snowboarding for various age cohorts. An X2 test was used to compare the differences between the two surgical department chair groups. Fisher’s exact test was conducted instead of an X2 test when more than 20 percent of cells had an expected count of less than five. * p < 0.05, ** p < 0.01, *** p < 0.001.
References
[expand title=”Click to View All”]1. O’Connor KL, Baker MM, Dalton SL, Dompier TP, Broglio SP, Kerr ZY. Epidemiology of Sport-Related Concussions in High School Athletes: National Athletic Treatment, Injury and Outcomes Network (NATION), 2011-2012 Through 2013-2014. J Athl Train. 2017;52(3):175-185.
2. Kearney PE, See J. Misunderstandings of concussion within a youth rugby population. J Sci Med Sport. 2017.
3. Statistic Brain Research Institute. Youth Sports Statistics. Sports 2017; https://www.statisticbrain.com/youth-sports-statistics/.
4. Hatfield DP, Chomitz VR, Chui KK, Sacheck JM, Brown AA, Economos CD. Impact of a Community-Based Physical Activity Program on Fitness and Adiposity Among Overweight and Obese Children. Health Promot Pract. 2016.
5. Colberg SR, Albright AL, Blissmer BJ, et al. Exercise and type 2 diabetes: American College of Sports Medicine and the American Diabetes Association: joint position statement. Exercise and type 2 diabetes. Med Sci Sports Exerc. 2010;42(12):2282-2303.
6. Hebert JJ, Klakk H, Moller NC, Grontved A, Andersen LB, Wedderkopp N. The Prospective Association of Organized Sports Participation With Cardiovascular Disease Risk in Children (the CHAMPS Study-DK). Mayo Clin Proc. 2017;92(1):57-65.
7. Daniels SR, Arnett DK, Eckel RH, et al. Overweight in children and adolescents: pathophysiology, consequences, prevention, and treatment. Circulation. 2005;111(15):1999-2012.
8. Fishman M, Taranto E, Perlman M, Quinlan K, Benjamin HJ, Ross LF. Attitudes and Counseling Practices of Pediatricians Regarding Youth Sports Participation and Concussion Risks. J Pediatr. 2017;184:19-25.
9. American Board of Neurological Surgery. Training Requirements. Board Certification 2017; https://www.abns.org/Board-Certification/Training-Requirements/July-2013/.
10. Accreditation Council for Graduate Medical Education. ACGME Program Requirements for Graduate Medical Education in Neurological Surgery. Chicago, IL: Accreditation Council for Graduate Medical Education;2017.
11. Accreditation Council for Graduate Medical Education. ACGME Program Requirements for Graduate Medical Education in Orthopaedic Surgery. Chicago, IL: Accreditation Council for Graduate Medical Education;2017.
12. Sweeney TE, Salles A, Harris OA, Spain DA, Staudenmayer KL. Prediction of neurosurgical intervention after mild traumatic brain injury using the national trauma data bank. World J Emerg Surg. 2015;10:23.
13. American Board of Physical Medicine and Rehabilitation. Brain Injury Medicine Examination Outline. Buffalo Grove, IL: American Board of Physical Medicine and Rehabilitation;2014.
14. Wijdicks EF, Rabinstein AA, Manno EM, Atkinson JD. Pronouncing brain death: Contemporary practice and safety of the apnea test. Neurology. 2008;71(16):1240-1244.
15. Uhl RL, Rosenbaum AJ, Czajka C, Mulligan M, King C. Minor traumatic brain injury: a primer for the orthopaedic surgeon. The Journal of the American Academy of Orthopaedic Surgeons. 2013;21(10):624-631.
16. Peterson AR, Kruse AJ, Meester SM, et al. Youth Football Injuries: A Prospective Cohort. Orthop J Sports Med. 2017;5(2):2325967116686784.
17. Rosene JM, Raksnis B, Silva B, et al. Comparison of Concussion Rates Between NCAA Division I and Division III Men’s and Women’s Ice Hockey Players. Am J Sports Med. 2017;45(11):2622-2629. [/expand]
[aans_authors]