You can never be overdressed or overeducated –
As if completing college, medical school and residency were not enough, three prominent neurosurgeons decided to pursue additional graduate education in the fields of business, public health and law. As part of our Back to School issue, this three-part series includes their experience. They share stories, explain their motivation, discuss what they learned and reflect on the value of their over-education.
Rather than going through a major mid-life crisis, I decided it might be best to go back to school when I turned fifty. I looked at all the options, including possibly doing an MBA, MPH or Master’s in Health Administration. I needed something that would be easily accessible, as I really did not want to leave my practice for a year or longer. I was not that keen on an MBA, since I wanted to sharpen my research perspective. I was also lukewarm on healthcare administration. After having practiced in Louisiana for over 20 years at that time, I was distraught about seeing so many hypertensive hemorrhages that could be prevented by taking medication that cost only a few cents per day. The other thing that alarmed me was that people with third grade educations and small cervical discs were undergoing extensive spinal operations. I felt these were unnecessary spinal surgeries and this was something I found deeply concerning.
I thought if I could do some sort of summer course or an online course, it might just help. Fortunately, that idea worked out well, for I went to the Harvard School of Public Health almost 9 years ago. It was a great and I called it my ‘Harvard ashram’ experience. It was nice to live in a small apartment. I would take a bike to school and be surrounded by people obviously brighter than myself and interact with them on a wide range of carnivorous topics, ranging from public health, social determinants, finances and management.
It was great to bicycle on the Charles, work out, go to the gym and stay up late reading a ton of papers that I would never have read. The best thing about this was that it was a rich intellectual interaction that definitely strengthened my perspective. Full disclosure, I was not so bad in math when I was in high school, but math at the age of 50 is a little bit more challenging than I thought it would be. In terms of requirements, since I hadn’t done the MCAT, I had to take the GRE and that was tolerable. My first semester was the hardest, because it was mainly statistics. I developed mathematical fatigue fairly rapidly. Thankfully, the rest of the courses were more fun. I really enjoyed courses about social determinants of health as well as management and ethics. Just a caution, this obviously was not cheap. The MPH cost about $25,000. During those semesters, I would tend to work for ten days, take a Friday off, go to clinic to operate on the weekends and then come back. Thus, I would be there for six weeks and would come back for two weekends. Fortunately, Laura, my wife, and our children were nearby at the New Jersey shore. I would take the Amtrak train on other weekends down to New Jersey and that worked out well.
So what did I learn? I think disseminations in health care take time and people are fairly resistant. One of the best examples is referenced in “Disseminating innovations in health care”; it took almost 150 years to implement lemon juice every day on sea voyages to help prevent scurvy.1 Historically, Florence Nightingale is considered one of the founders of public health because of her pie charts showing the mortality of the Crimean war hospitals. What we also saw was a disproportional distribution of healthcare, which was self-evident in terms of supply and demand. One thing was clear cut, that people with less resources have worse outcomes. This was fairly well documented. I knew this intuitively, but school provided proof.
I think the big issue was and still is the cost of health care, which was galloping to almost 20 percent of the Gross Domestic Product (GDP). We have very sound economists who say our health care costs have to be less than the cost of inflation. They also point out how poorly we do compared to other Organization for Economic Co-operation and Development (OECD) Countries. They shed light on the staggering differences in geographical disparities between laminectomy rates in different parts of the country or Medicare spending by state. In conclusion, I think the value of health care was something with which I was not acquainted. Michael Porter’s suggestion that quality and service divided by cost equals “value” was excellent and it helped me understand things, like disruptive innovations in healthcare.
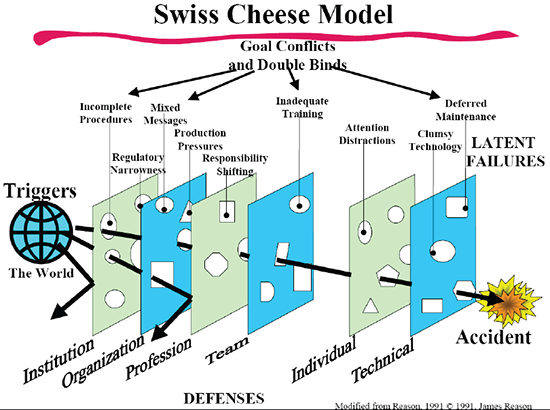
Lastly, I think the malpractice situation was discussed well at Harvard. The actual incidence is lower than we think, and it is interesting to see how other countries litigate medical issues. (In some countries, surgeons are killed for poor results.) Finally, the Swiss Cheese Model shows that mistakes can happen and that was clearly emphasized through examples in the aeronautical industry (Figure 1).
I believe public health has a wonderful and endearing way of reaching a far larger population on issues such as vaccinations, concussions or adding fluoride to the water. It was an intellectual feast for me and I strongly recommend it.
Figure 1: Swiss Cheese Model
References
1. Berwick, D. M. (2003). Disseminating innovations in health care. JAMA, 289(15), 1969–1975.