Editor’s Note: One obvious way to think about the world of neurosurgery is that it is the culmination of all the care delivered across the subspecialties. Just a few decades ago, subspecialization (and the whole world of CAST, enfolded fellowships, post-residency fellowships, etc.) was the exception, limited to just a small number of academics. Today it plays a much larger role across the neurosurgical spectrum. In a series of pieces, AANS Neurosurgeon explores each of the subspecialties in neurosurgery’s orbit.
The care of patients with central nervous system (CNS) tumors remains a challenging and complex undertaking, marked by frequent “promising” breakthroughs, but few that ultimately impact clinical management. The growing sophistication of diagnostic tests, chemotherapeutics and adjuvant medical management requires constant vigilance to an ever-increasing body of knowledge, with appropriate adaptation to each patient’s unique history and goals of care. The formalized field of neuro-oncology initially grew from collaborations between neurosurgeons, neurologists and oncologists, who recognized the need for dedicated teams to manage increasingly complex therapeutic regimens in medically challenging patients. Since the first brain tumor research meeting held in Asilomar in 1975, interest in the field of neuro-oncology has grown exponentially. Dedicated fellowships were developed in the 1980s, and a number of national societies were subsequently inaugurated, including the Japanese Society for Neuro-Oncology (1980), Korean Society for Neuro-Oncology (1991), European Association of Neuro-Oncology (1994) and the (American) Society of Neuro-Oncology (1996). Subsequently, these societies have provided an invaluable platform for dissemination of ideas, promotion of education and advancement of scientific research.
Progress in clinical neuro-oncology depends on a perpetual cycle of scientific discovery, clinical translation and pilot protocols, randomized trials (with either rejection or confirmation of the hypothesis) and treatment optimization in both the laboratory and the bedside – a process that can take a decade or more. Surgical excision remains the mainstay of treatment for most CNS neoplasms, with abundant, albeit non-randomized, evidence supporting its role. After controlling for other prognostic factors, early surgical resection results in better survival than watchful waiting in low-grade glioma1, and numerous studies have correlated extent of resection and long-term survival in both low and high grade glioma.2-4 In addition to therapeutic benefit, surgical excision provides tissue for pathologic studies, which is essential for selection of appropriate adjuvant therapies. Advancements in neurosurgical oncology have focused on optimizing extent of resection and include the ubiquitous adaptation of the operating microscope, the development of image-guided surgery and the use of intra-tumoral florescence using 5-aminolevulinic acid.5 Indeed, recent work continues to validate the role of extent of resection in the molecular age, with increased survival shown in maximally resected glioblastoma independent of IDH1 status.6 However, disagreement can exist among experts about the resectability of a given lesion7, and even complete resection is rarely curative.8
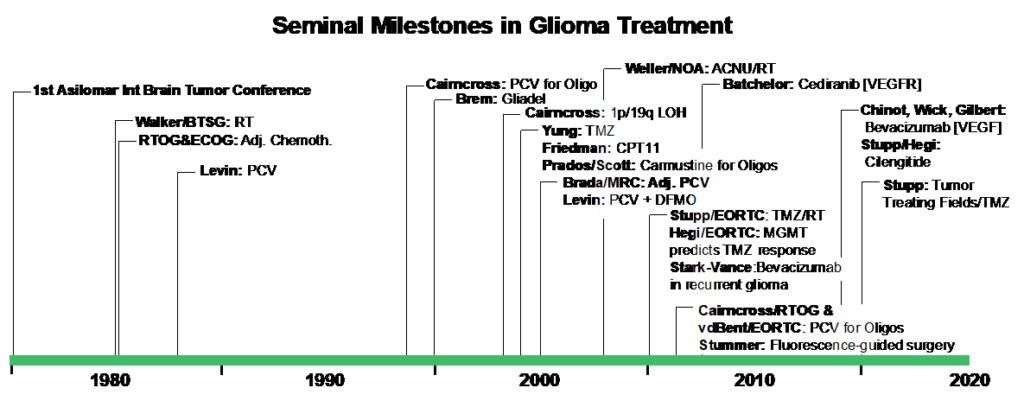
Seminal studies in neuro-oncology have transformed approaches to management and prognostication (Figure 1). For example, the use of adjuvant radiotherapy has become standard of care for most malignant lesions, following early studies that demonstrated benefit in high-grade gliomas.9 Considerable attention has also focused on the role of chemotherapy in CNS tumors, with numerous cytotoxic drugs and combinations being investigated and aiming to replicate the successes observed in medical oncology. Anaplastic oligodendrogliomas were among the first to be identified as truly chemo-sensitive tumors, exhibiting a durable response to combination therapy of procarbazine, lomustine and vincristine (PCV)10-11 or adjuvant carmustine.12 They are also responsive to radiation therapy and have a more protracted natural history irrespective of the treatment modality. Subsequently, the biology of oligodendroglioma has been associated with loss of chromosomes 1p and 19q (later identified as a translocation)13-14, and this genomic feature has become pathognomonic for these tumors.
Glioblastoma, the most common and deadly adult primary brain tumor, has been the subject of extensive research, though clinical outcomes remain overall dismal. Contemporary standard of care includes maximal surgical resection, followed by adjuvant radiation with concomitant and maintenance temozolomide (TMZ) chemotherapy.15-16 This strategy increased the two-year survival rate from 10% to 27%, though only 10% of patients remained alive after five years (compared to 3% who did not receive chemotherapy as part of the initial management).15 Notably, patient response to TMZ depends upon promoter methylation of the DNA repair gene O6-methylguanine–DNA methyltransferase17 (resulting in epigenetic inactivation). This predictive marker is now part of routine pathological assessment, allowing for better prognostication and individualization of the post-operative treatment strategy. Recent work has also investigated the use of concomitant tumor treating fields (TTFields), a novel treatment modality thought to disrupt cell division and organelle assembly. A large phase III trial demonstrated improved progression-free and overall survival when TTFields were added to standard maintenance TMZ chemotherapy early in the disease course.18-20
The notable progress made over the past four decades has not come without setbacks, with “promising” results from pre-clinical or phase I/II trials often failing to show efficacy in subsequent phase III trials. Prominent examples in glioblastoma include targeting VEGFR and VEGF by cediranib21-22 or bevacizumab23-24, Cilengitide25-26, as well as Rindopepimut and other EGFR inhibitors.27-28 A persistent challenge in the treatment of CNS tumors is the presence of a blood-brain barrier, which can reduce penetrance of drug therapy and thereby decrease efficacy. Recent work has investigated blood-brain barrier disruption using a variety of techniques, including radiation, ultrasound or osmotic agents29 and ongoing trials in humans will ultimately determine the utility of these approaches.30 The employment of surgery for localized delivery of chemotherapeutics has also shown promise, for example the intraoperative implantation of biodegradable carmustine (Gliadel) wafers.31 However, both concentration and extent of diffusion were insufficient to allow for a sustained antitumor effect. Current investigations are using oncolytic virus injection during surgical resection to improve regional control, change the immunological milieu and microenvironment or deliver cytotoxic agents, though preliminary analyses provide inconsistent results.32-35
As our understanding of tumor pathogenesis and progression continues to mature, clinical neuro-oncology has become an increasingly precise enterprise. Early studies on chemotherapeutics focused on large heterogeneous cohorts, segregated primarily by histological attributes such as putative cell of origin or presence of aggressive features. The advent and proliferation of molecular profiling has led to increasing disease stratification, with the goal of tailoring chemotherapeutics and specific genomic or epigenetic signatures. This new dimension of tumor profiling has also increased the accuracy of prognosis, facilitating optimal clinical management and expectation setting. Continued development of precision treatments, methods of earlier detection and diagnosis, along with finding an optimal balance between surgical and medical approaches, will further improve outcomes among patients with CNS tumors and likely serve as the foundation for future management of these patients.
References
[expand title=”View All”]
1. Jakola, A. S., Myrmel, K. S., Kloster, R., Torp, S. H., Lindal, S., Unsgård, G., & Solheim, O. (2012). Comparison of a Strategy Favoring Early Surgical Resection vs a Strategy Favoring Watchful Waiting in Low-Grade Gliomas. Jama, 308(18), 1881. doi: 10.1001/jama.2012.12807
2. Keles, G., Anderson, B., & Berger, M. S. (1999). The effect of extent of resection on time to tumor progression and survival in patients with glioblastoma multiforme of the cerebral hemisphere. Surgical Neurology, 52(4), 371–379. doi: 10.1016/s0090-3019(99)00103-2
3. Lacroix, M., Abi-Said, D., Fourney, D. R., Gokaslan, Z. L., Shi, W., Demonte, F., … Sawaya, R. (2001). A multivariate analysis of 416 patients with glioblastoma multiforme: prognosis, extent of resection, and survival. Journal of Neurosurgery, 95(2), 190–198. doi: 10.3171/jns.2001.95.2.0190
4. Ushio, Y., Kochi, M., Hamada, J.-I., Kai, Y., & Nakamura, H. (2005). Effect of Surgical Removal on Survival and Quality of Life in Patients With Supratentorial Glioblastoma. Neurologia Medico-Chirurgica, 45(9), 454–461. doi: 10.2176/nmc.45.454
5. Stummer, W., Pichlmeier, U., Meinel, T., Wiestler, O. D., Zanella, F., & Reulen, H.-J. (2006). Fluorescence-guided surgery with 5-aminolevulinic acid for resection of malignant glioma: a randomised controlled multicentre phase III trial. The Lancet Oncology, 7(5), 392–401. doi: 10.1016/s1470-2045(06)70665-9
6. Molinaro, A. M., Hervey-Jumper, S., Morshed, R. A., Young, J., Han, S. J., Chunduru, P., … Berger, M. S. (2020). Association of Maximal Extent of Resection of Contrast-Enhanced and Non–Contrast-Enhanced Tumor With Survival Within Molecular Subgroups of Patients With Newly Diagnosed Glioblastoma. JAMA Oncology. doi: 10.1001/jamaoncol.2019.6143
7. Sonabend, A. M., Zacharia, B. E., Cloney, M. B., Sonabend, A., Showers, C., Ebiana, V., … Mckhann, G. (2017). Defining Glioblastoma Resectability Through the Wisdom of the Crowd. Neurosurgery, 80, 590–601. doi: 10.1227/neu.0000000000001374
8. Levin, V. A. (1999). Chemotherapy for brain tumors of astrocytic and oligodendroglial lineage:The past decade and where we are heading. Neuro-Oncology, 1(1), 69–80. doi: 10.1093/neuonc/1.1.69
9. Walker, M. D., Green, S. B., Byar, D. P., Alexander, E., Batzdorf, U., Brooks, W. H., … Strike, T. A. (1980). Randomized Comparisons of Radiotherapy and Nitrosoureas for the Treatment of Malignant Glioma after Surgery. New England Journal of Medicine, 303(23), 1323–1329. doi: 10.1056/nejm198012043032303
10. Cairncross, G., Macdonald, D., Ludwin, S., Lee, D., Cascino, T., Buckner, J., … Schold, C. (1994). Chemotherapy for anaplastic oligodendroglioma. National Cancer Institute of Canada Clinical Trials Group. Journal of Clinical Oncology, 12(10), 2013–2021. doi: 10.1200/jco.1994.12.10.2013
11. van den Bent, M. J., Brandes, A. A., Taphoorn, M. J., Kros, J. M., Kouwenhoven, M. C., Delattre, J.-Y., … Hoang-Xuan, K. (2013). Adjuvant Procarbazine, Lomustine, and Vincristine Chemotherapy in Newly Diagnosed Anaplastic Oligodendroglioma: Long-Term Follow-Up of EORTC Brain Tumor Group Study 26951. Journal of Clinical Oncology, 31(3), 344–350. doi: 10.1200/jco.2012.43.2229
12. Prados, M. D., Scott, C., Curran, W. J., Nelson, D. F., Leibel, S., & Kramer, S. (1999). Procarbazine, Lomustine, and Vincristine (PCV) Chemotherapy for Anaplastic Astrocytoma: A Retrospective Review of Radiation Therapy Oncology Group Protocols Comparing Survival With Carmustine or PCV Adjuvant Chemotherapy. Journal of Clinical Oncology, 17(11), 3389–3395. doi: 10.1200/jco.1999.17.11.3389
13. Cairncross, J. G., Ueki, K., Zlatescu, M. C., Lisle, D. K., Finkelstein, D. M., Hammond, R. R., … Louis, D. N. (1998). Specific Genetic Predictors of Chemotherapeutic Response and Survival in Patients With Anaplastic Oligodendrogliomas. JNCI: Journal of the National Cancer Institute, 90(19), 1473–1479. doi: 10.1093/jnci/90.19.1473
14. Jenkins, R. B., Blair, H., Ballman, K. V., Giannini, C., Arusell, R. M., Law, M., … Buckner, J. C. (2006). A t(1;19)(q10;p10) Mediates the Combined Deletions of 1p and 19q and Predicts a Better Prognosis of Patients with Oligodendroglioma. Cancer Research, 66(20), 9852–9861. doi: 10.1158/0008-5472.can-06-1796
15. Stupp, R., Hegi, M. E., Mason, W. P., Bent, M. J. V. D., Taphoorn, M. J., Janzer, R. C., … Mirimanoff, R.-O. (2009). Effects of radiotherapy with concomitant and adjuvant temozolomide versus radiotherapy alone on survival in glioblastoma in a randomised phase III study: 5-year analysis of the EORTC-NCIC trial. The Lancet Oncology, 10(5), 459–466. doi: 10.1016/s1470-2045(09)70025-7
16. Stupp, R., Mason, W. P., Bent, M. J. V. D., Weller, M., Fisher, B., Taphoorn, M. J., … Mirimanoff, R. O. (2005). Radiotherapy plus Concomitant and Adjuvant Temozolomide for Glioblastoma. New England Journal of Medicine, 352(10), 987–996. doi: 10.1056/nejmoa043330
17. Hegi, M. E., Diserens, A.-C., Gorlia, T., Hamou, M.-F., Tribolet, N. D., Weller, M., … Stupp, R. (2005). MGMTGene Silencing and Benefit from Temozolomide in Glioblastoma. New England Journal of Medicine, 352(10), 997–1003. doi: 10.1056/nejmoa043331
18. Stupp, R., Taillibert, S., Kanner, A., Read, W., Steinberg, D. M., Lhermitte, B., … Ram, Z. (2017). Effect of Tumor-Treating Fields Plus Maintenance Temozolomide vs Maintenance Temozolomide Alone on Survival in Patients With Glioblastoma. Jama, 318(23), 2306–2316. doi: 10.1001/jama.2017.18718
19. Stupp, R., Taillibert, S., Kanner, A. A., Kesari, S., Steinberg, D. M., Toms, S. A., … Ram, Z. (2015). Maintenance Therapy With Tumor-Treating Fields Plus Temozolomide vs Temozolomide Alone for Glioblastoma. Jama, 314(23), 2535. doi: 10.1001/jama.2015.16669
20. Stupp, R., Wong, E. T., Kanner, A. A., Steinberg, D., Engelhard, H., Heidecke, V., … Gutin, P. H. (2012). NovoTTF-100A versus physician’s choice chemotherapy in recurrent glioblastoma: A randomised phase III trial of a novel treatment modality. European Journal of Cancer, 48(14), 2192–2202. doi: 10.1016/j.ejca.2012.04.011
21. Batchelor, T. T., Sorensen, A. G., Tomaso, E. D., Zhang, W.-T., Duda, D. G., Cohen, K. S., … Jain, R. K. (2007). AZD2171, a Pan-VEGF Receptor Tyrosine Kinase Inhibitor, Normalizes Tumor Vasculature and Alleviates Edema in Glioblastoma Patients. Cancer Cell, 11(1), 83–95. doi: 10.1016/j.ccr.2006.11.021
22. Batchelor, T. T., Duda, D. G., Tomaso, E. D., Ancukiewicz, M., Plotkin, S. R., Gerstner, E., … Jain, R. K. (2010). Phase II Study of Cediranib, an Oral Pan–Vascular Endothelial Growth Factor Receptor Tyrosine Kinase Inhibitor, in Patients With Recurrent Glioblastoma. Journal of Clinical Oncology, 28(17), 2817–2823. doi: 10.1200/jco.2009.26.3988
23. Chinot, O. L., Wick, W., Mason, W., Henriksson, R., Saran, F., Nishikawa, R., … Cloughesy, T. (2014). Bevacizumab plus Radiotherapy–Temozolomide for Newly Diagnosed Glioblastoma. New England Journal of Medicine, 370(8), 709–722. doi: 10.1056/nejmoa1308345
24. Gilbert, M. R., Dignam, J. J., Armstrong, T. S., Wefel, J. S., Blumenthal, D. T., Vogelbaum, M. A., … Mehta, M. P. (2014). A Randomized Trial of Bevacizumab for Newly Diagnosed Glioblastoma. New England Journal of Medicine, 370(8), 699–708. doi: 10.1056/nejmoa1308573
25. Stupp, R., Hegi, M. E., Gorlia, T., Erridge, S. C., Perry, J., Hong, Y.-K., … Weller, M. (2014). Cilengitide combined with standard treatment for patients with newly diagnosed glioblastoma with methylated MGMT promoter (CENTRIC EORTC 26071-22072 study): a multicentre, randomised, open-label, phase 3 trial. The Lancet Oncology, 15(10), 1100–1108. doi: 10.1016/s1470-2045(14)70379-1
26. Stupp, R., Hegi, M. E., Neyns, B., Goldbrunner, R., Schlegel, U., Clement, P. M., … Weller, M. (2010). Phase I/IIa Study of Cilengitide and Temozolomide With Concomitant Radiotherapy Followed by Cilengitide and Temozolomide Maintenance Therapy in Patients With Newly Diagnosed Glioblastoma. Journal of Clinical Oncology, 28(16), 2712–2718. doi: 10.1200/jco.2009.26.6650
27. Schuster, J., Lai, R. K., Recht, L. D., Reardon, D. A., Paleologos, N. A., Groves, M. D., … Sampson, J. H. (2015). A phase II, multicenter trial of rindopepimut (CDX-110) in newly diagnosed glioblastoma: the ACT III study. Neuro-Oncology, 17(6), 854–861. doi: 10.1093/neuonc/nou348
28. Weller, M., Butowski, N., Tran, D., Recht, L., Lim, M., Hirte, H., … Nag, S. (2017). Rindopepimut with temozolomide for patients with newly diagnosed, EGFRvIII-expressing glioblastoma (ACT IV): a randomised, double-blind, international phase 3 trial. The Lancet Oncology, 18, 1373-1385 doi: 10.1016/S1470-2045(17)30517-X
29. Sprowls, S. A., Arsiwala, T. A., Bumgarner, J. R., Shah, N., Lateef, S. S., Kielkowski, B. N., & Lockman, P. R. (2019). Improving CNS Delivery to Brain Metastases by Blood–Tumor Barrier Disruption. Trends in Cancer, 5(8), 495–505. doi: 10.1016/j.trecan.2019.06.003
30. Sonabend, A. M., & Stupp, R. (2019). Overcoming the Blood–Brain Barrier with an Implantable Ultrasound Device. Clinical Cancer Research, 25(13), 3750–3752. doi: 10.1158/1078-0432.ccr-19-0932
31. Westphal, M. (2003). A phase 3 trial of local chemotherapy with biodegradable carmustine (BCNU) wafers (Gliadel wafers) in patients with primary malignant glioma. Neuro-Oncology, 5(2), 79–88. doi: 10.1215/15228517-5-2-79
32. Cloughesy, T. F., Mochizuki, A. Y., Orpilla, J. R., Hugo, W., Lee, A. H., Davidson, T. B., … Prins, R. M. (2019). Neoadjuvant anti-PD-1 immunotherapy promotes a survival benefit with intratumoral and systemic immune responses in recurrent glioblastoma. Nature Medicine, 25(3), 477–486. doi: 10.1038/s41591-018-0337-7
33. Desjardins, A., Gromeier, M., Herndon, J. E., Beaubier, N., Bolognesi, D. P., Friedman, A. H., … Bigner, D. D. (2018). Recurrent Glioblastoma Treated with Recombinant Poliovirus. New England Journal of Medicine, 379(2), 150–161. doi: 10.1056/nejmoa1716435
34. Chiocca, E. A., Yu, J. S., Lukas, R. V., Solomon, I. H., Ligon, K. L., Nakashima, H., … Cooper, L. J. N. (2019). Regulatable interleukin-12 gene therapy in patients with recurrent high-grade glioma: Results of a phase 1 trial. Science Translational Medicine, 11(505). doi: 10.1126/scitranslmed.aaw5680
35. Reardon, D. A., Omuro, A., Brandes, A. A., Rieger, J., Wick, A., Sepulveda, J., … Sampson, J. (2017). OS10.3 Randomized Phase 3 Study Evaluating the Efficacy and Safety of Nivolumab vs Bevacizumab in Patients With Recurrent Glioblastoma: CheckMate 143. Neuro-Oncology, 19(suppl_3), iii21–iii21. doi: 10.1093/neuonc/nox036.071
[/expand]
[aans_authors]