The initial metamorphosis of health care reform focused on inequality and access. The future shift to cost containment is inescapable. In response to this, hospitals are merging and acquiring physician practices at an astounding rate (4). This began at the primary care level to give hospitals access to a pool of patients for referral and admittance. In other words, it created future customers. This practice has now expanded to surgical sub-specialties. The thought is fairly simple: the hospitals are going to gain control over the market so they can control more market power. Economic principles are working for the hospital. This decreases competition and will increase cost. It is in this context that neurosurgeons will need to continue to prove their value.
Gaining Market Power
Let’s look at more straightforward colloquial example. Let’s say Fed-Ex and UPS are engulfed in a battle for customers in Cambridge, Mass. During the summer months, the air conditioning unit at the UPS store breaks, and the employees demand a new central air conditioning system immediately at a substantial cost to the company. UPS management reluctantly agrees, thereby dramatically increasing the price of production. Their supply cost has increased, and they must pass this on to the consumer at possibly an additional $1 per package in order to stay open. Fed-Ex gets wind of this and drops its prices. This seems mildly counter-intuitive in that their main competitor just raised prices. In theory, Fed-Ex could still benefit from raising the price somewhere less than a dollar. Why did Fed-ex show restraint in raising the price? They want to gain market power.
They want to attract all the customers and have them get used to shopping in their store, using their mailboxes and knowing their delivery drivers. Fed-Ex waits because when Christmas time comes around, they will raise the price to $2. Sure, Fed-Ex may lose some customers, but they are starting off with more customers than they ever had before. In economics terms, they made the market more inelastic for demand. More importantly, they made the switch during a time frame when the consumer is not very price sensitive (2). No one wants to be renegotiating with Fed-Ex management on Dec. 23 about where the Christmas card deliveries should go and how much they should cost. The question then becomes when are hospitals, who are increasing their local market power, going to pull the rug out from under physicians and patients?
Could that moment be when we transform to a bundled or capitated payment structure? Instead of neurosurgeons serving as productivity based, relative work-value unit generators, they will function as a budget item. Raw salary will decrease from a profit standpoint. An independent neurosurgery group could combat this. The physicians hold bargaining power. The hospital would be forced to meet some of the physician demands or otherwise face losing the bundled payment altogether. However, as the hospitals merge, they gain more ammunition in their arsenal that turns into controlling the entire hospital market in the region.
Consolidation and Control, not Improvement
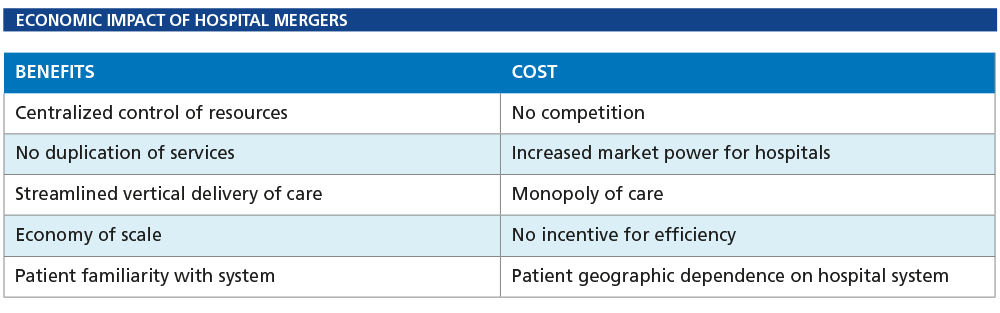
Hospital groups claim that mergers reduce cost by reducing the duplication of services. The data is just not supporting that (4). They further claim an economy of scale benefit in that a greater cost advantage with increased volume of services exists. Perhaps, but the more sinister side of me cannot see past their obvious benefit to control delivery of local healthcare at the patient level.
To the economist, hospital mergers largely represent local rent-seeking behavior. This perverts the economic system and sets up a sub-optimal allocation of resources. Rent-seeking behavior occurs when an organization or individual looks to increase their share of wealth without generating any new wealth (3). By merging, hospitals are taking up more of the market to increase their own wealth without explicitly generating more health-care delivery overall. They are not expanding care, and they are not deliberately improving care by merging. They are consolidating it.
Hospital mergers will attempt to set up barriers of access into the economic market that favor the hospital. It sets up an obvious monopoly of physical health resources, such as operating rooms, clinics, etc. It also creates a monopoly of patients. Some hospital systems are even creating their own insurance platforms. Mergers create a “guild” mentality that will locally exclude anyone who does not participate in the hospital’s particular system.
Hospitals have an enormous financial incentive to buy up their competition. In economics, incentives matter. Incentives change behavior. The very fact that something is being measured changes behavior patterns in anticipated and unanticipated ways (3). In Santiago, Chile, in response to long waiting times for bus passengers, the city created a per rider incentive for bus drivers. Wait times plummeted, yet accidents among hurried bus drivers increased 67 percent (2). Economics focuses on the scarcity of resources and opportunity cost. Each decision made is compared directly to the next possible alternative that is subsequently missed. Essentially, economics is about trade-offs; one opportunity is missed for another (3). Each merger changes local reform and value landscape. Neurosurgeons must be aware of that.
Getting Involved is Essential
Neurosurgeons have the unique ability to bring a unified voice to the local policy argument to ensure that the incentives created always favor the patient-physician relationship and not special interests. Again, each reform decision will come at the cost of another decision. Each hospital merger will come with intended and unintended consequences. Neurosurgeons need to be in those discussions to speak on behalf of the patient’s best interest.
Those not in the specialty are attempting to shape the value and delivery of neurosurgery. Hospital mergers will have an impact on future value determination and will certainly have an impact on the delivery of neurosurgery. Neurosurgeons need to make outcomes, quality and value a top priority because if we cannot provide our own metrics, another organization will create them for us (1).
To accomplish this, neurosurgeons must step out of the narrow corridor of focused rigorous scientific evaluation. We must step into the realm of economics and policy because that is the arena in which our value is being evaluated and manipulated. In short, it is neurosurgeons who actually take care of neurosurgical patients, not hospitals. Therefore, it is neurosurgeons that must continue to create a unified voice to lobby of behalf of our patients.
[aans_authors]
References
- 1. Asher AL, McCormick PC, Selden NR, Ghogawala Z, McGirt MJ: The National Neurosurgery Quality and Outcomes Database and NeuroPoint Alliance: rationale, development, and implementation. Neurosurg Focus 34:E2, 2013
- 2. Blaine B: Thinking Like an Economist. 2015. Adaptation from Lecture, Microeconomics, Harvard Kennedy School of Government, July 2015
- 3. Mankiw G: Principles of Economics. 6th edition.
- 4. Monopolizing medicine: Why hospital consolidation may increase healthcare costs | Medical Economics: Available: https://medicaleconomics.modernmedicine.com/medical-economics/content/tags/hospital-employment/monopolizing-medicine-why-hospital-consolidation-?page=full. Accessed 31 July 2015