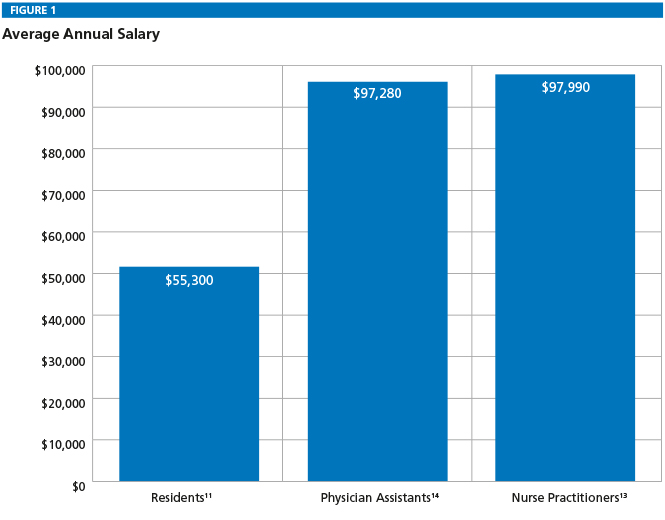
Since their implementation in 2003, the resident work-hour limitations have been widely criticized. While many of these dissensions have focused on the negative impact this policy has had on the medical education system, others have lamented the effect work-hour limitations have had on the productivity and finances of academic medical centers (AMCs) and their physicians. By limiting the resident work force, it has been argued, the educational, research, and clinical goals of these institutions have suffered and ultimately affected financial reimbursement, both at the institutional and individual provider level. To counter the mandates on resident work hours, alternative providers, “costly nurse practioners and physician assistants,” are required to fill the clinical gap. The salaries of these nonphysician providers can be double that of a resident for working “one-half of [the] hours” and seeing “one-half as many patients” (16) (Figure 1).
Although these views are not singular, deriding the current medical education system in hopes of reverting to the prior apprenticeship model is unlikely to be fruitful as resident work-hour limitations are now the reality of modern day academic medicine. These financial concerns, however, do raise the question of the value of resident physicians and the equality, or inequality, of their pay in comparison to the remainder of the clinical workforce. A clear answer requires an understanding of the complex system determining payments to hospitals participating in graduate medical education (GME) as well as deciphering how a residency program affects hospitals’ costs and efficiency of providing clinical care. As nebulous as Medicare’s GME payments are, the second issue is almost more difficult to unravel but obviously should have great impact on the level of support for operating residency programs and the financial reimbursement of house staff.
Graduate Medical Education Funding and Identifying the Value of Resident Education
Value is positively impacted by quality and service and is disproportional to cost and time. While the education of residents improves their quality and the service that they subsequently provide, these educational efforts are associated with substantial costs, as well as time and effort by educators and administrative staff. This reciprocal arrangement is even reflected in the legislation that created Medicare and the GME system.
In 1965, Congress identified the value of resident education and the need to more formally fund this process, noting, “…educational activities enhance the quality of care in an institution” (6). A portion of these educational funds were also intended to compensate hospitals for their increased costs as well as the “inefficiencies” created by the teaching of residents and the potentially costly care that they provide.
Exactly what the overall GME costs are appears difficult to fully quantify, and it is unclear how much Medicare’s payments alleviate these costs. A 2013 report to the Medicare Payment Advisory Commission determined that the annual mean GME cost per resident was $134,803, while a study of family medicine residents at the University of Washington calculated it to be significantly higher, at $338,421 (8). It is likely to be much higher in a more technical specialty like neurosurgery. The disparity in these figures characterizes the ambiguity in identifying GME costs accurately and thus supporting them adequately.
Crucial to the funding of the American GME system, is the value and cost of residents within academic medical centers. As stated above, Congress noted in 1965 that “educational activities enhance the quality of care in an institution,” but later in 1983, determined that this education was associated with “additional costs.” Is it therefore true that residents 1) improve care, but 2) are more costly than alternative health-care workers?
Do Residents Increase the Cost of Clinical Care?
The argument could be made that residents increase quality of care by serving as a significant component of the clinical workforce in tertiary medical centers, whose existence, or at least current level of functioning, wouldn’t be possible without a sufficient resident physician presence. They play a large role in providing this higher level of acute care, treating the uninsured and sustaining clinical research and technological improvements. Again, identifying the extent of this value is difficult.
Several studies have, however, compared the clinical care provided by teams employing residents against those of non-teaching services (i.e., attending physicians alone or in some combination with nurse practitioners or physician assistants). In comparable settings, patients cared for by teaching services typically had comparable or improved clinical outcomes (e.g., length of stay, inpatient mortality, readmission rates), similar hospital charges and in one study even had higher patient satisfaction scores (7, 15, 17, 20, 22). Through these measures, it does not appear that resident care is the “cost-inefficient” endeavor that Congress proposed that it was.
The efficiency and cost of the additional measures specifically dedicated to the education of residents is unclear. With stricter guidelines outlining education curriculums and mandates for closer supervision of resident staff, it may be possible that the time dedicated to resident teaching by attending physicians may limit clinical and academic productivity. The converse may instead be true, however, in that the efforts of residents may actually free staff of some clinical responsibilities and ultimately make them more effective. Thus, with residents performing some of the more routine tasks of clinical care, patient volume both in the outpatient clinics and in the operating room may be increased and more time may also be allotted to academic activities.
Resident Compensation
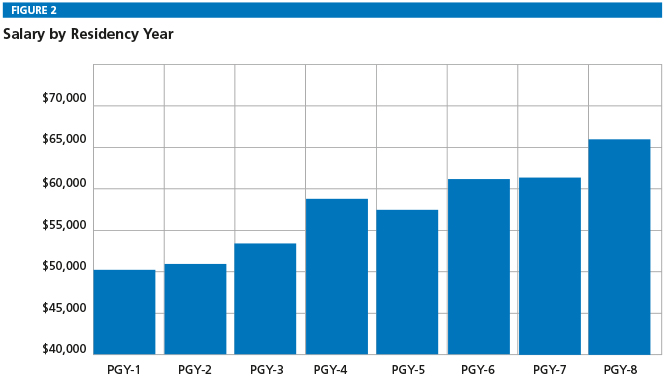
The mean salary for a PGY-1 resident in the United States is $50,765 and incrementally increases each subsequent year to a mean of $66,261 for PGY-8 residents (1) (Figure 2). Although this number has increased modestly with time, minimal resources have been dedicated to increasing resident compensation in the past. In fact, when adjusted for inflation, resident salaries have not changed in 40 years (21). As a result, resident indebtedness has increased more rapidly than inflation (6) (Figure 3). The consequences of these financial constraints and hardships on the developing physician work force are severe. During training, residents may spend time moonlighting, leading to exhaustion and the potential for deterioration in the care provided. Additionally, residents may be encouraged to pursue more lucrative specialties and avoid the lower pay of primary care or research. Finally, promising students may be dissuaded from the pursuit of medicine as an occupation due to these financial limitations. The public health repercussions in an increasingly aging population may be devastating.
 Upon completion of residency training, where heavy financial debt is incurred and minimally, if at all, offset by limited salaries, physicians may be forced to seek suboptimal, but high-paying, positions. The sacrifice of working long hours with heavy patient loads in undesirable locations may be necessary to maximize financial earning. This may contribute to the nearly 40 percent of physicians suffering from symptoms of burnout (19). This figure is likely higher in the surgical specialties, potentially leading to poor clinical performance and patient outcomes (18).
Upon completion of residency training, where heavy financial debt is incurred and minimally, if at all, offset by limited salaries, physicians may be forced to seek suboptimal, but high-paying, positions. The sacrifice of working long hours with heavy patient loads in undesirable locations may be necessary to maximize financial earning. This may contribute to the nearly 40 percent of physicians suffering from symptoms of burnout (19). This figure is likely higher in the surgical specialties, potentially leading to poor clinical performance and patient outcomes (18).
Increasing residents’ pay may limit some of the above concerns. The cost of such a measure for each of the 110,000 residents in training in the U.S. would be substantial, however. For example, an additional $25,000 annually, per resident, would result in an additional $2.75 billion added to a health-care system that already spends $2.8 trillion per year (4). Sustaining any increase in resident salary would likely not be possible in the current system. Instead, it has been suggested that the current GME system be redesigned to re-appropriate such funds rather than simply expanding the current costs (4, 5). Others have advocated for private insurers to contribute further to graduate medical education payments as well.
Conclusion
The societal benefit of resident education is indisputable. The need for well-trained, competent and technically skilled future physicians is critically important, particularly with an increasingly aging population. In turn, sufficient support — educational, supervisory and financial — is necessary to foster and maximize the graduate medical education system.
Resident physicians are critical to the functioning of academic medical centers and their provision of higher-level care, a fact that has been widely recognized even in the legislation that serves to fund these institutions. Additionally, multiple studies have shown that residents likely make this care more efficient and effective. This value currently goes unrecognized in our current GME system, a fault that is reflected in residents’ low salaries. This has significant repercussions on the subsequent motivations of house staff in their attempts to “make up ground” financially, resulting in decisions that may have wide-sweeping effects on public health care.
To close that gap and sufficiently reimburse resident staff, a substantial overhaul of the system designed for GME support may be required. This would be concordant with the modern paradigm shift in medical reimbursement towards an emphasis on value-driven care. In an updated, improved system, the value of the resident physician would be recognized and sufficiently compensated.
[aans_authors] References
9. MedPAC Report to Congress: Aligning Incentives in Medicare. June 2010
21. Sunshine J. The residents rise up. Medical Examiner Slate.com https://www.slate.com/articles/health_and_science/medical_examiner/2014/05
/medical_residents_pay_doctors_in_training_are_organizing_for_collective.html Accessed July 15, 2014.